Acute Pelvic Inflammatory Disease (PID)
Definition: It is the polymicrobial infection and inflammation of the upper genital tract typically involving the fallopian tubes, ovaries and surrounding structures (endometritis, salpingitis, pelvic peritonitis, tubo-ovarian abscess).
Causative organisms:
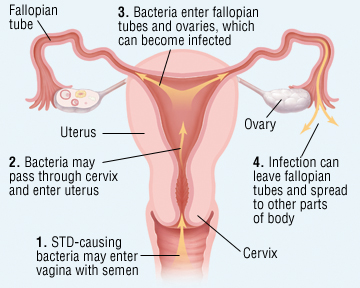
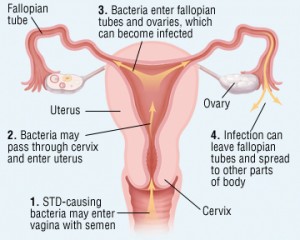 Primary organisms: Ascending spread of micro-organisms from cervico-vaginal canal
Primary organisms: Ascending spread of micro-organisms from cervico-vaginal canal
- Neisseria gonorrhoeae (1/3rd cases)
- Chlamydia trachomats (1/3rd cases)
- Mycoplasma hominis (1/10th cases)
Secondary organisms:
- Endogenous aerobes: Non-hemolytic streptococcus, E.coli, Group B streptococcus, Staphylococcus
- Endogenous anaerobes: Bacteroides, Peptostreptococcus, Peptococcus
Risk Factors:
- Young, nulliparous, sexually active women with multiple sex partners for whom we also recommend this hiv test kit
- Douching
- Prior PID
- IUD use
- Iatrogenic procedures: Endometrial biopsy, Uterine curettage, Hysterosalpingography
Protective Factors:
- Contraceptive: OCPs and Barrier methods
- Menopausal, pregnant with monogamous partner
Symptoms:
- Lower abdominal and pelvic pain (dull)
- Fever and chills
- Nausea and vomiting (indicates peritonitis)
- Menstrual disturbances
- Purulent cervical discharge
- Dyspareunia
- RUQ pain indicates perihepatitis (Fitz-Hugh-Curtis syndrome)
Signs:
- Vitals: Elevated temperature > 38c
- Abdominal palpation: Bilateral lower abdominal tenderness
- Vaginal examination:
- Purulent vaginal discharge
- Congested external urethral meatus or openings of Bartholin’s ducts
- Speculum examination: Congested cervix with purulent discharge
- Bimanual examination:
-
- Chandelier sign: Cervical motion tenderness
- Adnexal tenderness
- Thickening or definite mass
Minimum clinical criteria for diagnosis
- Cervical motion tenderness
- Uterine tenderness
- Adnexal tenderness
The presence of temperature higher than 38.3° C (101° F) and abnormal cervical or vaginal mucopurulent discharge enhance the specificity of the minimum criteria, as do selected laboratory tests.
Investigations and Diagnosis:
- Identification of organisms:
- Endocervical swabs (Gram stain and culture)
- Urine microscopy and culture
- Lab:
- WBC > 10,000/cu.mm
- ESR > 15mm/hr
- Raised CRP
- Serological test for syphilis: on both partners
- Ultrasonography: To rule out tubo-ovarian abscess
- Laparoscopy: To rule out appendicitis or ectopic pregnancy and to aspirate fluid for analysis
- Indicated if diagnosis is uncertain or failure to respond to antibiotic therapy within 48-72 hours
- Laparotomy: It is strongly recommended if
- Patient > 40 years
- Recurrent PID attacks
- History of tubal ligation
- Other:
- Saline microscopy of cervical or vaginal discharge
- B-hCG: To rule out pregnancy (ectopic pregnancy)
- Pelvic CT and MRI (not routinely recommended)
Differential diagnosis:
- Acute appendicitis
- Adnexal torsion (Ovarian torsion)
- Diverticulitis
- Ectopic pregnancy
- Endometritis
- UTI
Adler sign: For distinguishing appendicitis from adnexal or uterine pain, if the point of maximal tenderness shifts medially with repositioning on the left lateral side, etiology is generally gynecologic
Complications:
- Immediate: Pelvic/Generalized peritonitis, Septicemia
- Late: CDEF
- Chronic PID
- Chronic pelvic pain
- Dyspareunia
- Ectopic pregnancy
- Fertility impaired (Infertility)
Treatment:
All sex partners examined and treated appropriately
Outpatient antibiotic therapy: Oral therapy
- Regimen A: Cefoxitin 2gm im + Probenecid 1gm oral X 1 dose
- Regimen B: Ceftriaxone 250 mg im X 1dose + Doxycycline 100mg BD X 14 days
- Regimen C: Ofloxacin 400 mg bd + Metronidazole 500 mg X 14 days
Inpatient antibiotic therapy: IV therapy
- Indications: PID
- Pelvic abscess
- Pregnancy
- Immunodeficient: HIV or Immunosuppresive
- Intolerance or Unresponsive to Outpatient antibiotic therapy
- Illness: Severe illness, high fever
- Diagnosis uncertain: Surgical emergencies (ectopic pregnancy and acute appendicitis) cannot be ruled out
- Regimen A: Cefoxitin 2gm iv 6 hrly OR Cefotetan 2gm iv 12 hrly + Doxycycline 100 mg iv or orally 12 hrly X 14 days
- Regimen B: Clindamycin + Gentamycin X 14 days
Surgery:
- Tubo-ovarian abscess:
- NG tube, IV fluids, Investigations
- Antibiotics: Ofloxacin 400 mg iv 12 hrly + Metronidazole 500 mg orally or iv 8 hrly OR Imipenem 500 mg iv 6 hrly
- Surgical excision
- Transcutaneous/Transvaginal aspiration
- Overwhelming infection or Chronic intractable pelvic pain:
- Hysterectomy and BSO
Follow up:
- Repeat smears and cultures after 7 days of discharge
- Repeat following each menstrual period until it becomes negative for 3 consecutive reports
Gainesville staging of Acute PID:
- Stage I: Acute endometritis-salpingitis without peritonitis
- Stage II: Acute salpingitis with peritonitis
- Stage III: Acute salpingitis with superimposed tubal occlusion
- Stage IV: Ruptured tubo-ovarian abscess or tubo-ovarian complex
- Stage V: Respiratory complications
Therapeutic goals:
- Stage I: Eliminate symptoms and infectivity
- Stage II: Preservation of fallopian tube function
- Stage III: Preservation of ovarian function
- Stage IV: Preservation of patient’s life
For Stage III and IV: An antimicrobial cover with at least 3 drugs i.e., beta –lactam, clindamycin and tobramycin, should be provided. If there is a deterioration in the patient’s condition, rupture of an abscess should be considered and surgical exploration is recommended.
Simple and straight to the point, thank you
Great stuff…used it for osce
excellent summary. much appreciated
simplified and adequate.