Staphylococcus Aureus : Lab Diagnosis and Diseases
STAPHYLOCOCCUS:
Classification:
Family: Micrococcacea
Genus: Micrococcus and Staphylococcus
Species: S.aureus, S.epidermidis, S.saprophyticus, M.luteus, etc.
Streptoccaceae and Micrococcacea both are family of gram positive cocci.
1. Streptococcacea : Catalase negative
2. Micrococcacea : Catalase positive
Based on coagulase production, micrococcacea are:
a. Coagulase positive: S.aureus
b. Coagulase negative: S.epidermidis, S.saprophyticus
Micrococcus is strictly anaerobic, form irregular clusters or tetrads and do not ferment glucose whereas staphylococcus is normally facultative anaerobe and ferments glucose.
| Test | S. aureus | S. epidermidis | S.saprophyticus |
| Coagulase | Positive | Negative | Negative |
| Novobiocin sensitivity | Sensitivie | Sensitive | Resistant |
| Acid from mannitol fermentation anaerobically | Positive | Negative | Negative |
| Phosphatase | Positive | Positive | Negative |
STAPHYLOCOCCUS AUREUS:
Morphology: Gram positive, non-sporing, non-motile, usually non-capsulate, aerobic and normally facultative anaerobic cocci (1micrometer in diameter) arranged in grape-like clusters.
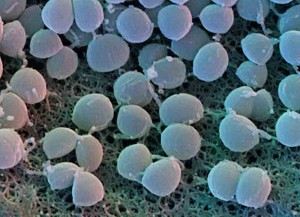
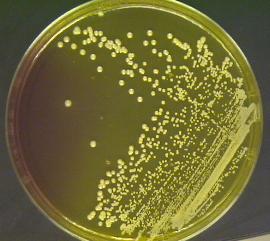
Colony characteristics: large, round, smooth, raised, shiny, opaque and are often pigmented with deep yellow pigment.
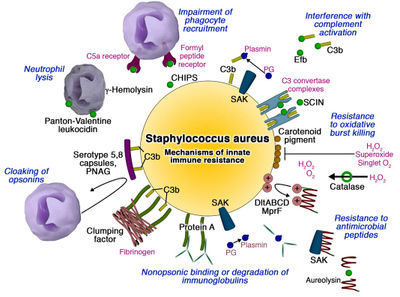
VIRULENCE FACTORS:
a. Strucutural components:
i. Capusle: Present in some strains lacking bound coagulase
– inhibits chemotaxis and phagocytosis
– inhibits proliferation of mononuclear cells
– facilitates adherence to foreign bodies
ii. Peptidogycan:
– Evokes production of IL-1 (endogenous pyrogen having endotoxin like activity) and opsonic antibodies by monocytes
– Leukocyte chemoattractant
iii. Protein A: It is a surface protein covalently bound to the peptidoglycan layer
– Inhibits antibody mediated clearance by binding with IgG1, IgG2 and IgG4 Fc receptors
– Leukocyte chemoattractant
– Anticomplementary
b. Toxins:
i. Exotoxins:
a. Enterotoxins (A to F) : staphylococcal food poisoning
b. Toxic shock syndrome toxin-1 (TSST-1): produce leakage or cellular destruction of endothelial cells
ii. Leukocidins (P-V) : kills polymorphonuclear leukocytes and macrophages
iii. Hemolysins (alpha, beta, gamma, delta): lyse erythrocytes
iv. Exfoliative toxins (ETA, ETB): split the stratum corneum leading to separation and loss of most superficial layers of the epidermis
c. Enzymes:
i. Catalase: catalyzes removal of hydrogen peroxide
ii. Coagulase: converts fibrinogen to fibrin
iii. Hyalurinidase: hydrolyzes hyaluronic acid in tissue, promoting the spread of staphylococci
iv. Fibrinolysin: dissolve fibrin clots
v. Lipases
vi. Nucleases
vii. Penicillinases
viii. Phosphatases
ix. Proteases
Most human strains produce coagulase A. The coagulase exists in 2 forms: free and bound
a. Free coagulase:
– Extracellular
– Heat labile
– Requires CRF(coagulase reacting factor- present in rabbit and human plasma but absent in guinea pigs) for clotting
– Tube test
b. Bound coagulase:
– Constituent of cell wall
– Heat stable
– Independent of CRF for reacting with fibrinogen
– Slide test
Production of bacteriocins by staphylococci is controlled by gene in plasmid.
LABORATORY DIAGNOSIS:
Specimens: Pus/discharge from supparative lesions, CSF from meningitis, blood from septicaemia, sputum from respiratory infection, and suspected food, vomit or faeces from food poisoning, needle aspiration
Culture:
i. Nutrient agar (non diffusible golden yellow pigment)
ii. Blood agar (usually beta hemolysis)
iii. Selective media like Ludlam’s media containing 8 to 10% NaCl (inhibits growth of most organisms other than staphylococci)
iv. Mannitol salt agar (fermented by S.aureus but not most of other staphylococci)
Biochemical tests:
a. Catalaste positive (helps to differentiate between Staphylococcus and Streptococcus)
b. Mannitol fermentation test (acid production without gas – usually by Staphylococcus aureus)
c. Phosphatase test (S. aureus positive, S epidermidis negative)
d. Coagulase test (differentiate coagulase positive and negative) – tube test and slide test
e. Most strain hydrolyse urea, reduce nitrates to nitrites, liquefy gelatin and MR, VP positive but indole negative.
f. Bacteriophage typing (a set of over 28 bacteriophage usied in typing)
g. PCR
h. Antibiogram pattern and Antibiotic sensitivity test (Penicillin-Cloxacillin-Vancomycin-Teicoplanin)
Identification:
a. Coagulase positive
b. Protein A formed by more than 95% strains
c. Phosphatase enzyme produced which is detected by culturing on nutrient agar containing phenolphthalein diphosphate.
d. DNA hydrolyzing deoxyribonuclease
e. Mannitol formation with acid production
f. Reduction of potassium tellurite to tellurium when grown in medium containing potassium tellurite.
PATHOGENESIS:
About 20-30% of healthy people carry the organisms in anterior nares; less often in skin, axilla and perineum; and mucous membrane of throat. Staphylococci are also found regularly on clothing, bed linens and other fomites in human environment.
The pathogenic capacity of a given strain of S.aureus is the combined effect of extracellular factors, virulence factors(as discussed earlier) together with invasive properties of the strain.
| Group | Lesions |
| Superficial infections | |
| Skin | Folliculitis. Boil, impetigo(pyoderma), carbuncle, abscess, styes, pemphigus, neonatarum, sepsis in wounds and burns |
| Deep infections | |
| Bone & joint
Respiratry tract Intestinal Cardiac CNS Blood stream Muscle |
Osteomyelitis & Brodie’s abscess, septic arthritis, bursitis
Tonsilitis, pharyngitis, pneumonia, lung abscess, empyema Enterocolitis Endocarditis, pericarditis Meningitis, brain abscess Septicaemia, pyaemic abscesses Pyomyositis |
| Toxin-mediated | |
| Toxic food poisoning
Staphylococcal scalded skin syndrome (SSSS) |
Nausea, vomiting, diarrhea due to ingestion of preformed toxin
Exfoliation of epidermis, blisters (rupturing), exposure of dermis, fever Fever, hypotension, vomiting, diarrhea, erythematous rash, hyperaemia |
Patient will come with either:
• Pain and swelling in the infected area, painful movement ,discharge and abscess
• Accompanied by other complaints and symptoms
ANTIBIOTIC SENSITIVITY:
Sensitive to: flucloxacillin, erythromycin, lincomycin, vancomycin and cephalosporins
Resistance to:
a. Penicillin: Developed resistance due to beta-lactamase production, change in MRSA
b. Multi drug resistance (MDR): due to drug resistance genes present in plasmids
Is it ok to use your pictures and diagram in an esay for my micro class. I will sure cite eveyy thing?
Thanks,
Doaa
Sure
What is likelihood that gram stain negative s. Aureus in late infection of total hip replacement would increase likelihood of congestive heart failure? My otherwise healthy 77year old father had diagnosis of s. Aureus last week (with survey) 8 days ago and 2 days ago, they identified congestive heart failure. Should a cardiologist do diagnostic testing for colonization in heart? If so, what test? His MDs don’t. Seem especially proactive. Or is my emotional involvement clouding my perception. He is on IV oxacillin, post-culture for the s. Aureus & lassie for CHF. Thanks.
I cannot provide you Medical Advice.
For Information Only-
Coagulase negative Staph is common infection after total hip replacement. There are many causes of Heart failure post-operatively.( Infection, fluid overload, PE etc) There is no Gram negative S. Aureus.
Following links may be helpful.
http://www.georgetownuniversityhospital.org/blank.cfm?id=555795
I don’t recommend you to rely on any internet advice for such medical problems.
Doc, i think you forget to include oral cavity infection as one of Staphylococcus aureus field of spread infection,it is a major cause of dental caries beside staphylococcus mutans..what do you think?
Streptococcus mutans play important role in tooth decay. The presence of staphylococcus as a resident oral flora is controversial. But now there is a growing evidence that suggest that staphylococci can be isolated from oral cavity. They cause angular cheilitis, endodontic infections, osteomyelitis of jaw, parotitis, oral mucositis. Their relation with Dental caries has also been displayed recently.