CARDIOGENIC PULMONARY EDEMA
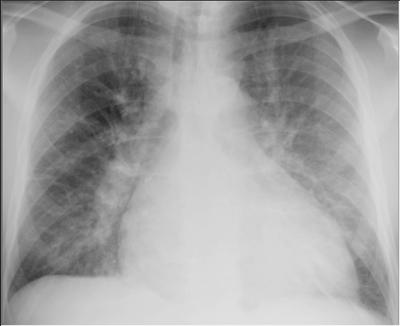
CARDIOGENIC PULMONARY EDEMA
DEFINITION:
Interstitial edema, including fluid engorgement of the perivascular and peribronchial spaces and the alveolar wall interstitium.
ETIOLOGY:
Arrhythmias , MI , severe systemic hypertension
Pulmonary embolism , valvular heart disease
Increased pulmonary capillary wedge pressure
PATHOPHYSIOLOGY:
Cardiogenic pulmonary edema occurs when the pulmonary capillary pressure exceeds the forces that maintain fluid within the vascular space (serum oncotic pressure and interstitial hydrostatic pressure).
Increased pulmonary capillary pressure may be caused by LV failure of any cause , obstruction to transmitral flow (mitral stenosis, atrial myxoma) or rarely pulmonary veno-occlusive disease.
Accumulation of fluid in the pulmonary interstitium is followed by alveolar flooding and impairment of gas exchange.
DIAGNOSIS:
CLINICAL PRESENTATION:
Signs and Symptoms:
Dyspnea, increased respiratory rate,
Cough with expectoration( pink frothy sputum)
Cyanosis , anxiety, restlessness, nocturnal dyspnea
Physical signs of decreased peripheral perfusion, pulmonary congestion (rales) , use of accessory respiratory muscles and wheezing.
IMAGING AND DIAGNOSTIC STUDIES:
Chest X-ray findings:

Prominent pulmonary vessels: interstitial and perihilar vascular engorgement, abnormal distension of upper lobe pulmonary veins, right and left pulmonary arteries dilate
Cardiomegaly: enlarged cardiac silhouette
Kerley B line: interstitial edema causes thickened interlobular septa and dilated lymphatics; these are evident as horizontal lines in the costophrenic angles.
Pleural effusions
Reticular shadowing: hazy opacification spreading from hilar region due to alveolar edema
Arterial Blood Gases:
Decreased partial pressure of arterial oxygen (PaO2).
Early on: normal to decreased partial pressureof arterial CO2 (PaCO2) , serum bicarbonate and respiratory alkalosis.
Late stages: increased PaCO2 , serum bicarbonate and respiratory acidosis.
ECG: to determine if arrhythmia is contributing to the development of pulmonary edema.
TREATMENT
Initial Management
-Supplemental oxygen(high flow, high concentration) should be administered initially to raise the arterial oxygen tension to >60mm Hg. Non-invasive positive pressure ventilation (continuous positive airway pressure CPAP, of 5-10 mm Hg) by a tight fitting face mask results in more rapid improvement.
-Placing the patient in sitting position reduces pulmonary congestion and improves pulmonary function.
-Strict bed rest, pain control, and relief of anxiety can decrease cardiac workload.
-Mechanical ventilation is indicated if oxygenation is inadequate by noninvasive means or if hypercapnia coexists.
-Precipitating factors should be identified and corrected.
MEDICATIONS:
sympathetically mediated peripheral vasoconstriction thus dilates pulmonary and systemic veins.
-Morphine 2-5 mg IV , can be given over several minutes and can be repeated every 10-25 minutes until an effect is seen.
Furosemide a loop diuretics is a venodilator that decreases pulmonary congestion within mins of IV administration. 20-80 mg IV should be given over several minutes.
Nitroglycerin IV is preferable to reduce preload and potentiate the effect of furosemide.
Nitroprusside is effective in treatment of CPE that results from valvular regurgitation or HTN.
Inotropic agents such as dobutamine or phosphodiesterase inhibitors may be helpful in patients with concomitant hypotension or shock.
Digoxin if in atrial fibrillation.
Recombinant BNP (nesiritide) administered as IV bolus followed by an IV infusion. Nesiritide reduces intracardiac filling pressures by producing vasodilation and indirectly increases the cardiac output.

1 Comment
The installation of asbestos is outlawed but a majority of complexes predating the particular prohibit have got massive measures coating the particular walls as well as ceilings as a flame resistent heat retaining material. Several different kinds of asbestos are viewed pretty secure when in tact however the moment it turns into damaged or actually starts to age; it could possibly relieve deadly fibres in the air causing deadly disorders such as Mesothelioma cancer or maybe Asbestosis.
Comments are closed.