Vernal Keratoconjunctivitis – VKC or Spring Catarrah
It is (RIBSA) Recurrent Interstitial Bilateral Self-limiting Allergic inflammation of the Conjunctiva having a Seasonal incidence. It is an hypersensitivity reaction to exogenous allergen specially grass pollen. IgE mediated reaction has a crucial role here.
Predisposing factors and Risk factors-
- Patient may have family history of atopic disease- hay fever,asthama,allergic rhinitis, atopic dermatitis. Their eosinophil count may be high in blood.
- Age- specially 4-20 years. Boys > girls
- Season- Summer is the main season “ warm weather conjunctivitis” . Spring Catarrah is known to be a misnomer.
- More prevalent in tropical areas than tundra region.
Symptoms-
- Marked burning and itching sensation in eyes – intolerable and aggravated by warm and humid condition.
- Mild Photophobia
- Ropy discharge ( string like)
- Lacrimation
- Heaviness of lids.
Signs-
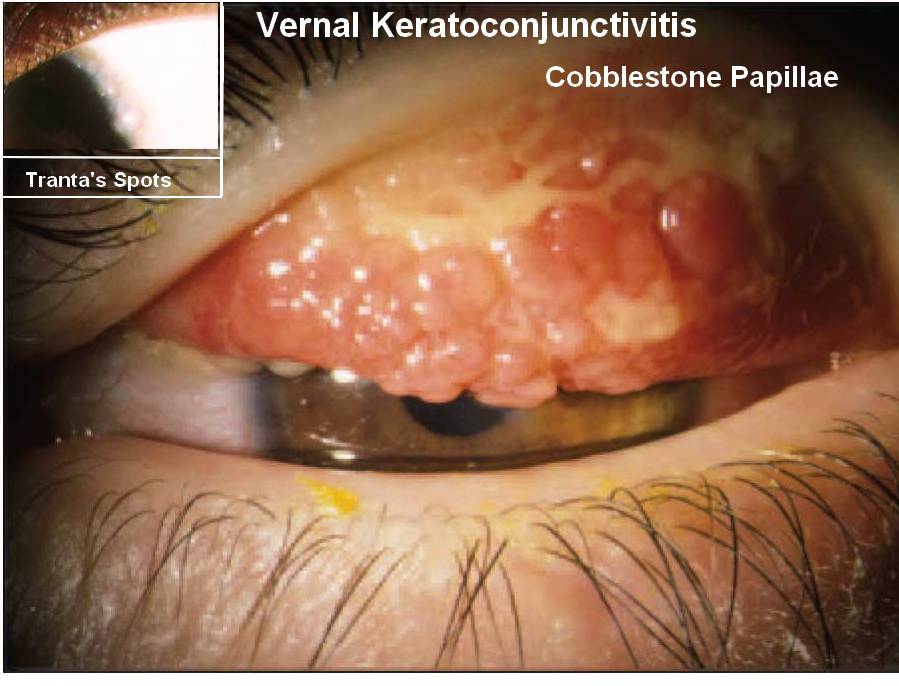
Palpebral form- Cobblestone or pavement stone arrangement of inflamed papillae on the Upper Tarsal conjunctiva. Cauliflower like giant papillae can be seen in extreme cases. White ropy discharge.
Bulbar form- Characterized by (DGTal– Mnemonic Dusky red triangle, Gelatinous accumulation, Tranta’s Spot)
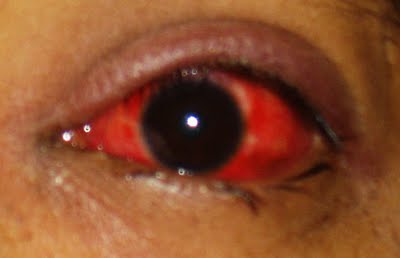
- Dusky red triangular congestion of the bulbar conjunctiva in palpebral area.
- Gelatinous accumulation aroung the limbus ( junction of cornea and conjunctiva)
- Tranta’s spot- discrete white dots along the limbus.
Mixed form. Features of both.
Vernal Keratopathy- Corneal lesions
PUS PV- Punctate Epithelial Keratitis, Ulcerative vernal Keratitis, Subepithelial scarring,Pseudogerontoxon, Vernal cornela plaques.
Prognosis- Disease is usually self-limiting and resolves in 5-10 years but may result in complications like Keartoconus.
Treatment-
General Measures-
- Dark goggles
- Cold compression
- Extreme cases shifting to a colder region may be necessary
Local-
- Topical Steroids – Q4hrly for 2 days then Q6-8hrly for 2 weeks
- Mast Cell stabilizer- Sodium cromoglycate 2 % drops 4-5 times a day, Azelasine drops.
- Topical Antihistaminics
- Acetyl Cysteine 0.5% used a muclytic .
- Topical Cyclosporine 1% in severe and unresponsive cases.
Systemic therapy-
- Oral antihistaminics
- Oral steroids
Treatment of large papillae-
- Supratarsal injection of long acting steroid
- Cryo-application
- Surgical excision.
Reference: Ophthalmology- A K Khurana, Web

2 Comments
I have 3 year old bouy with severe VKC. I realy need to hear from somone hwo have this disease or is taking care of child with this.
Please send me an e-mail kth@islandia.is
In my country doctors are not familiar to this desease.
best regards
Kristin Th
Hello Christine, if you are still not helped by someone please contact me in my Skype Chris.alex70
Comments are closed.