Electromyography
EMG: Introduction, Uses, Preparation, Procedure, Diagnoses and Risks
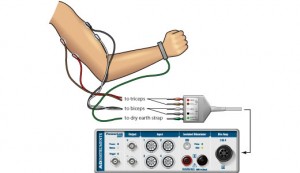
Electromyography (EMG) is a medical test performed to evaluate and record the electrical activity (electromyogram) produced by skeletal muscles using an instrument called electromyograph. EMG test is often performed together with another test called nerve conduction study, that measures the conducting function of nerves.
The electrical source is the resting membrane potential (RMP) which is about -90 mV for skeletal muscles. Measured EMG potentials range between less than 50 μV and up to 20 to 30 mV depending upon the muscle under observation.
You can also make an appointment with a reliable service provider similar to Freya’s Laser & Body Sculpting for an electrical muscle stimulation (EMS) that refines and tones muscles almost all over the body. It enhances muscle strength and endurance while aiding in the breakdown of fat, making this non-invasive body treatment a highly demanded one. Check out The Body Sculpting Institute for online body contouring certification courses.
Use of EMG:
- To find diseases that damage muscle tissue, nerves, or the neuromuscular junctions. eg. ALS, Myasthenia Gravis (MG)
- To find the cause of weakness, paralysis, or muscle twitching.
Preparation for EMG:
- Taking medicines that act on nervous system (anticholinergics) and blood thinners (warfarin) should be stopped before the test.
- Smoking should be avoided atleast for 3 hours before the test.
- Food and drinks containing caffeine should be avoided 2-3 hours before the test.
- Creams and lotions should be avoided on the day of test.
- Loose-fitting clothes add to ease and comfort for the test.
Procedure:
There are 2 types of EMG:
a. Intramusuclar EMG
b. Surface EMG
a. Intramuscular EMG:
- Regarded as invasive procedure.
- A needle electrode is inserted through the skin into the muscles.
- The electrical activity while inserting the electrode is observed. Normal muscles at rest make certain, normal electrical sounds when the needle is inserted into them.
- The electrical activity when the muscle is at rest is studied.
- The patient is asked to contract the muscle smoothly.
- The shape, size, and frequency of the resulting motor unit potentials are judged.
- Then the electrode is retracted a few millimeters, and again the activity is analyzed until at least 10–20 units have been collected.
b. Surface EMG:
- A surface electrode may be used to monitor the general picture of muscle activation, as opposed to the activity of only a few fibres as observed using a intramuscular EMG.
Normal Result:
Muscle tissue is normally electrically silent at rest. Once the muscles quiet down after the needles are inserted, there should be little muscle cell electrical activity noted on the screen.
When the muscle is voluntarily contracted, activity begins to appear. As contraction is increased, more and more muscle fibers produce action potentials until a disorderly group of action potentials of varying rates and amplitudes appears with full contraction.
Diagnoses from abnormal result:
Trauma Causes
- Traumatic peripheral neuropathy
- High cord injury
- Spinal cord transection/traumatic
- Congenital muscular dystrophy (Fukuyama type)
- Kubelberg Welander syndrome
Infectious Disorders (Specific Agent)
- Tetanus
- Post-Poliomyelitis syndrome
- Poliomyelitis, paralytic, spinal
- Poliomyelitis, paralytic, bulbar
- Vaccine associated paralytic polio
- Poliomyelitis, acute
- Viral Myopathy
Infected organ/Abscesses
- Myositis, inclusion body
Neoplastic Disorders
- Malignancy/cancer
- Metastasis to spinal cord
- Carcinomatous myopathy syndrome
- Opsoclonic-myoclonic/paraneoplastic syn
- Paraneoplastic myelitis/ANS neuropathy syndrome
Allergic, Collagen, Auto-Immune Disorders
- Guillain-Barre syndrome
- Dermatomyositis
- Dermatomyositis/childhood type
- Eaton-Lambert syndrome
- Mixed connective tissue disease (MCTD)/Undifferentiated
- Polymyositis
- Isaacs potassium channel myopathy syndrome
- Myositis synthetase syndrome/Anti-Jo-1 syndrome
Metabolic/Storage Disorder
- Diabetic amyotrophy syndrome
- Infantile mitochondrial myopathy/Cox defect
Congenital, Developmental Disorders
- Amyotonia, congenita
- Poliodystrophy/congenital
- Slow Channel Myasthenic Syndrome
Hereditary, Familial, Genetic Disorders
- Duchenne’s Muscular Dystrophy/Pseudohypertrophic
- Erb’s Muscular Dystrophy/Limb Girdle MD
- Muscular dystrophy, limb girdle type
- Muscular dystrophy, progressive
- Spinal muscle atrophy
- Spinal muscle atrophy, infantile
- Juvenile spinal muscle atrophy (Kugelberg-Welander)
- Kennedy Muscular atrophy disease
- Mitochondrial myopathy/MERRF
- Myhre Syndrome
- Distal muscular dystrophy (Gowers)
- Facioscapulohumeral muscular dystrophy
- Kearns-Sayre Ophthalmoplegic Syndrome
- Muscular atrophy, infantile, spinal
- Myotonia atrophica (Steinert’s disease)
- Myotonia congenita (Thomsens d.)
- Nemaline myopathy
- Oculopharyngeal muscular dystrophy
- Progressive spinal muscular atrophy
- Spinal muscle atrophy/adult type IV
- Muscular Dystrophy, Oculogastrointestinal type
- Myopathy, Myotubular/Centronuclear
Usage/Degenerative/Necrosis/Age/Related Disorders
- Muscle atrophy
- Amyotrophic lateral sclerosis (ALS)
- Primary lateral sclerosis
- Progressive bulbar palsy (Duchenne)
- Batten-Turner Muscular dystrophy
Anatomic/Foreign Body/Structural Disorders
- Spinal cord compression
- Suprascapular Nerve Entrapment
Arteriosclerotic/Vascular/Venous Disorders
- Spinal cord infarction
Vegetative/Autonomic/Endocrine Disorders
- Hypothyroidism (myxedema)
- Myasthenic crisis
- Myasthenia gravis
- Myasthenic syndrome (Pseudomyasthenia)
- Neonatal myasthenia
Reference to Organ System
- Motor peripheral neuropathy
- Neuromuscular disturbances/disorders
- Spinal cord lesion
- Motor neuron disease
- Radicular neuropathy
- Myopathy/secondary/nonspecific
- Peripheral neuropathy syndrome
Idiopathic/Unclassified Disorders
- Stiff-man syndrome
Pathophysiologic
- Motor denervation pathophysiology
Heirarchical Major Groups
- Muscle disorders
Drugs
- Steroid myopathy
- Drug induced Myopathy
Poisoning (Specific Agent)
- Alcohol myopathy
Organ Poisoning (Intoxication)
- Drug induced Neuromuscular junct/block
Risks:
- Mild discomfort and pain
- Mild shock
- Minimal bleeding
- Minimal risk of infection at the site of electrode insertion
Sources:
Diagnosispro
Wikipedia
Medlineplus
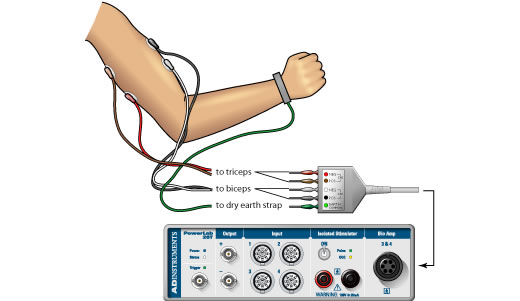
I believe surface and intramuscular are reversed
Thank you for informing about the error. It has just been corrected.