Brachial Plexus And Its Injury
 Definition:
Definition:
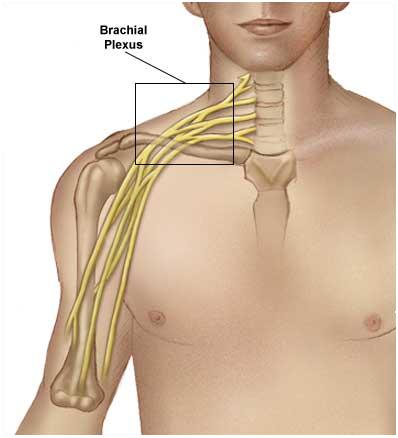
A network of spinal nerves that originates in the back of the neck, extends through the axilla (armpit), and gives rise to nerves to the upper limb. The brachial plexus is formed by the union of portions of the 5th through 8th cervical nerves (C5-C8) and the first thoracic nerve (T1), all of which come from the spinal cord.
Function:
The brachial plexus is responsible for cutaneous and muscular innervation of the entire upper limb, with two exceptions:
- the trapezius muscle innervated by the spinal accessory nerve (CN XI)
- an area of skin near the axilla innervated by the intercostobrachial nerve
Anatomy:
The plexus consists of roots, trunks, divisions, cords and branches.
Brachial plexus Mnemonic: Real (Root) Teen (Trunk) Drinks (Division) Cold (Cord) Beer (Branch)
- The roots lie between the anterior and middle scalene muscles.
- The trunks traverse the posterior triangle of the neck.
- The divisions lie behind the clavicle.
- The cords lie in the axilla.
a. Roots: The five roots are derived from the anterior primary rami of C5, 6, 7, 8 and T1. It also recieves contribution from anterior primary rami of C4 and T2. Depending on this there are 2 types of plexus:
- Prefixed: Contribution by C4 is large and that from T2 is often absent
- Postfixed: Contribution by T1 is large, T2 is always present, C4 is absent and C5 is reduced in size.
b. Trunks: These roots link up to form 3 trunks:
- Superior or upper (C5 and C6)
- Middle (C7)
- Inferior or lower (C8 and T1)
c. Divisions: Each trunk then splits in 2 (ventral and dorsal divisions), to form 6 divisions:
- Anterior divisions of the upper, middle, and lower trunks
- Posterior divisions of the upper, middle, and lower trunks
d. Cords: These 6 divisions will regroup to become the 3 cords. The cords are named by their position with respect to the axillary artery.
- Posterior cord: from the union of all 3 posterior divisions
- Lateral cord: from the fused anterior divisions of the upper and middle trunks
- Medial cord: from the anterior division of the lower trunk
e. Branches:
The cords continue distally to form the main nerve trunks of the upper limb, thus:
- Lateral cord continues as the musculocutaneous nerve
- Medial cord, as the ulnar nerve
- Posterior cord, as the radial nerve and the axillary nerve
- Cross-communication between the lateral and medial cords forms the median nerve
Median nerve supplies LOAF muscles in hand
- Lumbricals ( 1st and 2nd)
- Opponens pollicis
- Abductor pollicis brevis
- Flexor pollics brevis
Median nerve gives following cutaneous supply in hands:
- Lateral 3 and 1/2 on palamar side
- Middle 3 fingers on dorsal side
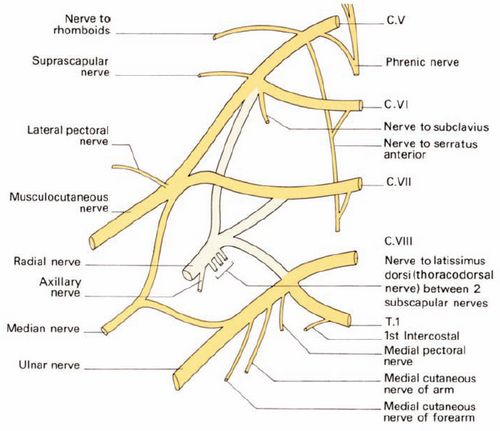
The derivatives of brachial plexus are:
From the roots
- Nerve to rhomboids (Dorsal scapular nerve) – C5
- Nerve to serratus anterior (Long thoracic nerve) – C5,C6 and C7
From the trunk
- Nerve to subclavius from the upper trunk – C5 and C6
- Suprascapular nerve from the upper trunk (supplies supraspinatusand infraspinatus) – C5 and C6.
From the lateral cord
Mnemonic: LML
Root of origin: C5, C6, C7
- Musculocutaneous nerve (coracobrachialis, brachialis and biceps brachi, lateral cutaneous nerve of forearm)
- Lateral pectoral nerve (pectoralis major)
- Lateral root of median nerve
From the medial cord
Mnemonic: MMMMU
Root of origin: C8, T1
- Medial pectoral nerve (pecotralis major and minor)
- Medial cutaneous nerves of arm and forearm
- Ulnar nerve (flexor carpi ulnaris, the medial 2 bellies of flexor digitorum profundus, most of the small muscles of the hand including 3rd and 4th lumbricals, the skin of the medial side of the hand and medial 1 and 1/2 fingers on the palmar side and medial 2 and 1/2 fingers on the dorsal side)
- Medial root of median nerve
From the posterior cord
Mnemonic: ULTRA
- Subscapular nerves (subscapularis and teres major) – C5, C6
- Nerve to latissimus dorsi (thoracodorsal nerve) – C6, C7, C8
- Axillary nerve (deltoid muscle, teres major, upper lateral cutaneous nerve of arm) – C5, C6
- Radial nerve (brachialis, brachioradialis, extensor muscle of forearm, anconeus, supinator, triceps, posterior cutaneous nerve of the arm) – C5, C6, C7, C8 and T1
Mnemonic: Radial Nerve Supplies BEAST muscles (brachialis, brachioradialis, extensor muscle of forearm, anconeus, supinator, triceps)
Note that the posterior cord supplies the skin and muscles of the posterior aspect of the limb whereas the anteriorly placed lateral and medial cords supply the anterior compartment structures.
Clinical Anatomy:
It may be damaged in open, closed or obstetrical injuries, be pressed uponby a cervical rib or be involved in tumour. It is encountered, and hence putin danger, in operations upon the root of the neck.
There are 4 types of brachial plexus injuries:
1. Avulsion: most severe type, in which the nerve is torn from the spine
2. Rupture: the nerve is torn but not at the spinal attachment
3. Neuroma: the nerve has tried to heal itself but scar tissue has grown around the injury, putting pressure on the injured nerve and preventing the nerve from conducting signals to the muscles
4. Neurapraxia or stretch: the nerve has been damaged but not torn. Neurapraxia is the most common type of brachial plexus injury.
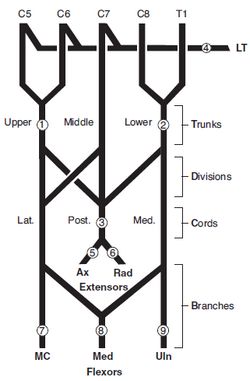 Lesions of Brachail Plexus: Bird’s Eye View
Lesions of Brachail Plexus: Bird’s Eye View
Correlate the numbers below with the numbers in the picture to find the part involved:
- Waiter’s tip (Erb’s palsy)
- Total claw hand (Klumpke’s palsy)
- Wrist drop
- Winged scapula
- Deltoid paralysis
- Saturday night palsy (wrist drop)
- Difficulty flexing elbow,variable sensory loss
- ↓ thumb function (“ape hand”)
- Intrinsic muscles of hand,claw hand (“Pope’s blessing”)
Erb’s Palsy:
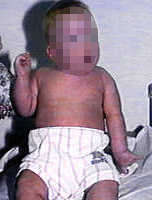
Site of injury: Erb’s point (meeting point of 6 nerves in upper trunk)
Causes: Undue separation of the head from the shoulder commonly encountered in: birth injury, fall of the shoulder or during anaesthesia
Nerve roots involved: C5, C6
Muscles paralysed: Mainly biceps, deltoid, brachialis and brachioradials. Partly supraspinatus, infraspinatus and supinator.
Deformity (Position of the limb): The deformity is known as ‘policeman’s tip hand’ or ‘porter’s tip hand’.
a. Arm: hangs by the side; it is adducted and medially rotated
b. Forearm: extended and pronated
Disability:
a. Abduction and lateral rotation of the arm
b. Flexion and supination of the forearm
c. Biceps and supinator jerks are lost
d. Sensations are lost over a small area over the lower part of deltoid.
Klumpke’s Paralysis:

Site of injury: Lower trunk of the brachial plexus
Cause of injury: Undue abduction of the arm, as in clutching something with hands after a fall from a height, or sometimes in birth injury.
Nerve roots involved: C8, T1
Muscles Paralysed:
a. Intrinsic muscle of the hand (T1).
b. Ulnar flexors of the wrist and fingers (C8).
Deformity (position of the hand):
a. Claw hand due to the unopposed action of the long flexors and extensors of the fingers.
b. In a claw hand there is hyperextension and the metacarpopharyngeal joints and flexion at the interphalangeal joints.
Disability:
- Claw hand.
- Cutaneous anaesthesia and analgesia in a narrow zone along the ulnar border of the forearm and hand.
- Horner’s syndrome: ptosis, mitosis, anhydrosis, enopthalmos, and loss of ciliospinal reflex- may be associated. This is because of injury to sympathetic fibers to the head and neck that leave the spinal cord through nerve T1.
- Vasomotor changes: The skin areas with sensory loss is warmer due to arteriolar dilation. It is also due to the absence of sweating as there is loss of symphatetic activity.
- Trophic changes: Long-standing case of paralysis leads to dry and scaly skin. The nails crack easily with atrophy of the pulp of fingers.
Injury to the Nerve to Serratus Anterior (Nerve of Bell):
Causes:
a. Sudden pressure on the shoulder from above.
b. Carrying heavy loads on the shoulder may cause shoulder pain and even lead to an injury to the Nerve to Serratus Anterior.
Deformity:
a. Winging of the scapula i.e. excessive prominence of the medial border of the scapula.
b. The pull of the muscle keeps the medial border against thoracic wall.
Disability:
a. Loss of pushing and punching actions. During attempts and pushing, there occurs winging of the scapula.
b. Arm cannot be raised beyond 90° i.e. overhead abduction which is performed by the serratus anterior is not possible).
Injury to Lateral Cord:
Cause: Dislocation of humerus.
Nerves involved:
a. Musculocutaneous
b. Lateral part of median nerve
Muscles paralysed:
a. Bicpes and coracobrachialis.
b. All muscles supplied by the median nerve, except those of the hand.
Deformity and disability:
a. Midprone forearm.
b. Loss of flexion of forearm.
c. Loss of flexion of the wrist.
d. Sensory loss on the radial sode of the forearm.
e. Vasomotor and trophic changes as above.
Carpal Tunnel Syndrome:
It is a syndrome characterized by the compression of the median nerve as it passes beneath the flexor retinaculum in carpal tunnel. Read more Carpal Tunnel Syndrome: Features and Treatment | Medchrome
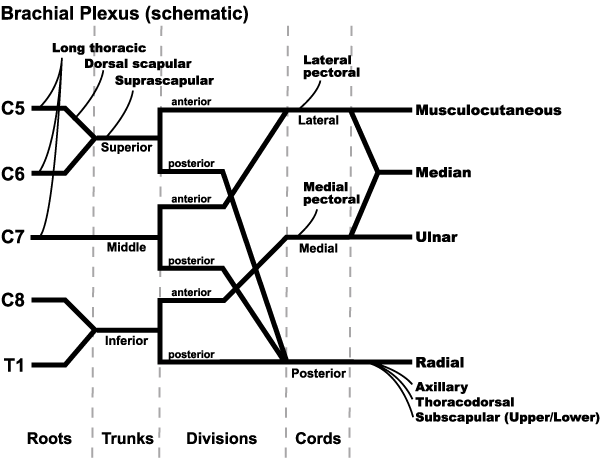
Drawing Brachial Plexus:
Learn to draw well labelled diagram of brachail plexus in 5 minutes
Great article am so glad that I found it. I am 34 and have had this now for about a month it’s June 2015 I have all above symptoms but have to say that the pain I’m in is horrible the worse I have ever been in and I have been through a spinal cord injury which I had major surgery back in 2008 which after i had to learn to walk again it was on my lower spine L3 and l4.because of this i have a condition called caude equine syndrome_”type of cronic pain” so I am already on a lot of medication for this type of nerve injury so nothing is working have not slept anyway I hope that the pain will ease up soon or I will go insane.
Great article. Concise and accurate.
Hi… very informative… my new born baby has Erb’s Palsy and Klumpke’s Paralysis symptons… can u pls gimme more info on this… will my baby recover and what treatment should I consider… also how long will it take for her to recover.
Great article.
Thanks
Have had A brachial plexus injury since 1973 Have use of my hand and fingers which took 24 months to start working at 90% No use of my arm at all.Pain never goes away feels like my arm and hand are on fire most of the time. Was 19 at the time of injury riding A bike and struck A light pole when nearly ran over by A car. Dr’s at UC Davis Cal could not correct back then by surgery sorry to say.Now days surgery can correct nerves that are torn out of the spine. Lucky to have good movement in my hand and fingers. But like I said the pain never stops have to take strong pain med’s 24 7 to have the best life I can
Carl
i have a bracial plexus injury to my left arm arising from a motorcycle accident in 1997,i have not had any surgery and have had severe pain for 3 years after the accident but i don’t take any medication and only have a mild pain constantly,the extreme pain subsided,i have no use of any part of my left arm,but i do have sensation to my elbow,its a terrible injury,is there any new technology in surgery to repair any of the arms movement these days?any help would be great.
Your story is similar to mine, I also had my accident in 1997 but mines the right arm, I lost complete use of it and have feeling to my elbow just like you, but the big difference is that my pain never went away, I wish mine had subsided like yours did after 3 years but unfortunately it’s always there, I take heavy pain meds to help control it but there are days when even all the pain meds in the world wont even put a dent in it, thankfully it only gets that bad a few times a year. If anyone knows of any new treatments I’d really like to hear about it.
Pain, numbness, and tingling in the fingers are all symptoms of carpal tunnel syndrome. Seeking medical treatment quickly could mean the difference between medications and surgery. If you’re having pain any of these carpal tunnel syndrome symtomps you should take action right away before it’s too late. A new keyboard or chair might let you live longer!