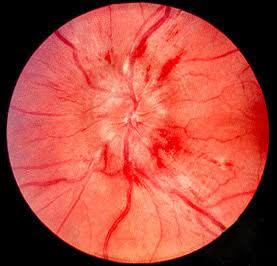
Transient vision loss
Background:
In adults, transient vision loss (TVL) is a frequently encountered complaint that, in most cases, has an identifiable cause. Transient vision loss may be monocular or bilateral and may last from seconds to hours. Episodes are often ischemic in origin, but other, more benign, conditions should be considered in the differential diagnoses (eg, dry eye, migraine). Causes of ischemic transient vision loss include giant cell arteritis, cerebrovascular ischemia, and retinal arteriolar emboli. Some authors refer to ischemic transient vision loss as amaurosis fugax syndrome. Transient vision loss can be a symptom of a serious vision or life-threatening condition, requiring urgent investigation and treatment, or it may have a more benign origin (eg, migraine, dry eye).
Transient vision loss in children is less common than in adults and is more likely to have a benign origin. Causes of bilateral transient vision loss in children include migraine and, less commonly, epileptic seizure.
Transient vision loss is a symptom rather than a diagnosis. It may be a manifestation of a number of different ophthalmic and systemic conditions.
Etiology:
The etiology of transient vision loss includes the following:
- Local ocular conditions
- Ingestion of a large meal
- Exercise
- Entopic phenomena.
- Elevated intracranial pressure (ICP).
- Minor head injury (occipital trauma).
- Familial factors.
- Migraine.
- Ocular treatments (intravitreal injections, trabeculectomy).
- Transient vision loss has been reported to occur after ingestion of a large meal.Visual loss occurs secondary to hypoperfusion of the eye, as blood is shunted to the mesenteric system. Postprandial visual loss is most common in individuals whose ocular perfusion is already compromised (eg, carotid disease, giant cell arteritis).
- Floaters – These may be due to posterior vitreous detachment or vitreous hemorrhage or may be from the normal vitreous.
Clinical picture:
N.B
Because of the many causes of transient visual disturbance, a structured approach to both the assessment and the management of these patients is essential. The likely causes of transient vision loss (TVL) vary according to the age of the patient. Ischemic causes are more common in patients older than 45 years; however, cases of CRAO and CRVO have been reported in children.
Any precipitating factors for the visual loss should be elicited. For example, visual loss related to orthostatic changes may occur in patients with papilledema. The patient should be asked about the specific nature of the disturbance. Ischemic visual disturbances, such as amaurosis fugax, are classically associated with negative phenomena (eg, a blackout of vision or a curtain across the vision). Migraine tends to produce positive phenomena (eg, sparkling lights or zigzag lines).
Associated symptoms may provide important clues to the etiology. Adults should be specifically asked about the symptoms of giant cell arteritis. Children should be asked about headaches and specifically about features of headaches that may suggest raised intracranial pressure (ICP) or migraine.
Physical examination:
The examination should look for ocular and systemic causes of the visual disturbance, as follows:
- Check the pupils for a relative afferent pupillary defect.
- Examine the visual fields, perform a cover test, and examine extraocular motility.
- Examine the eye; transient visual disturbance may be caused by intermittent angle-closure glaucoma, corneal disease (eg, corneal ulcers, corneal abrasions), or uveitis
- Perform dilated funduscopy; this may reveal optic disc edema, retinal emboli, or ocular ischemia.
- If pain is present, look for its specific causes (eg, angle-closure glaucoma, optic neuritis, or optic disc edema, suggesting increased IOP
Neuroimaging studies:
Although transient vision loss in children is most often benign, a serious underlying cause should be excluded. If symptoms are medically unexplained, clinical judgment should be used in deciding on appropriate circumstances for neuroimaging studies and further investigations.
Neuroimaging studies should be considered in the following:
- History of recent head trauma
- Focal neurological deficits
- Papilledema
- Proptosis
- Limited eye movement
Treatment & Managment:
The treatment of transient vision loss (TVL) depends on the cause. Some treatments for migraines, such as triptans, ergots, and betas, are avoided in migraines-induced transient vision loss owing to concern of worsening vasoconstriction.
If an ischemic event is suspected, then the patient should be referred to a physician for investigation of any cardiovascular and cerebrovascular risk factors. A retrospective study from Japan showed 2.9% of patients admitted for TIA presented with transient vision loss. Some of these patients benefit from antithrombotic therapy or carotid surgery. If the transient vision loss is monocular, the carotid system should be investigated, usually via carotid Doppler ultrasonography.
Other investigations may include echocardiography, a complete blood count (to rule out anemia), and inflammatory markers when giant cell arteritis is suspected. Neuroimaging is important for ruling out intracranial pathology affecting the visual pathway, particularly in patients with binocular disturbance. Empiric antiplatelet therapy (eg, daily aspirin) may be indicated while the evaluation is in progress for transient vision loss in patients with vasculopathy.
References:
1- Burde RM. Amaurosis fugax. An overview. J Clin Neuroophthalmol. 1989 Sep. 9(3):185-9. [Medline].
2- Meyer E, Gdal-On M, Zonis S. Transient monocular blindness in a case of drusen of the optic disc. Ophthalmologica. 1973. 166(5):321-6. [Medline].
3- Kunkel RS. Migraine aura without headache: benign, but a diagnosis of exclusion. Cleve Clin J Med.
Author bio.:
Mostafa. M. H. Haredi is a 4th year medical student in Minya Uni., Egypt.
He says – “I am a member in EMSA (Egyption Medical Students Association) which aims to help students to learn and how to research. I have published a question bank book for veterinary students and perparing for a clinical spots in anatomy. I’d like to help anyone want to know and learn”.