Understanding Medical Genetics
Clinical Genetics deals with the diagnosis of genetic diseases, care and counseling of patients with genetic disorders. Cytogenetics is the study of number & structure of chromosomes.
Common Terminologies:
- Genome: complete set of genes of a species
- Proband/Index case: an individual of family who draws an attention to physician for being genetic disorders
- Genotype: genetic constitution of an individual
- Phenotype: observable characteristic of an individual
- Dominant: a trait expressed in heterogygotes
- Recessive: trait is expressed only in homozygous and not in heterozygous
- Mutation: a permanent and heritable change in genetic material
- Expressivity: variation in the severity of a genetic trait
- Exon: coding region of a gene
- Introns: noncoding part of a gene
- Gene: DNA sequence which produces a functional polypeptide Or RNA.
- Allele: Alternative forms a gene at the same locus on a homologous chromosome.
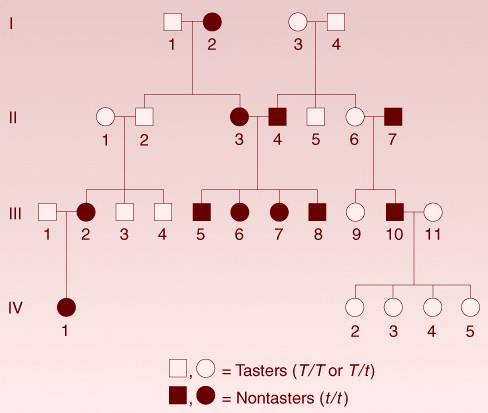
- Pedigree: diagrammatic representation of a family history important for the diagnosis of genetic diseases.
Classification of Genetic Disorders:
A) Single Gene Disorders (Mendelian)
- These are caused by mutant genes
- Single critical error in genetic information
- Exhibit obvious and characteristic pedigree pattern
B) Chromosomal Disorders
C) Multifactorial disorders
- Combined effect of various genes and environment can produce or predispose to a serious defect. e.g.: Glaucoma, cleft lip, neural tube defect, CHD, cancer and diabetes mellitus.
Mendelian Law of Inheritance:
- Law of Segregation: Each of the two inherited factors (alleles) possessed by the parent will segregate and pass into separate gametes (eggs or sperm) during meiosis, which will each carry only one of the factors.
- Law of Independent Assortment: In the gametes, alleles of one gene separate independently of those of another gene, and thus all possible combinations of alleles are equally probable.
- Law of Dominance: Each trait is determined by two factors (alleles), inherited one from each parent. These factors each exhibit a characteristic dominant; co-dominant, or recessive expression, and those that are dominant will mask the expression of those that are recessive.
Inheritance:
- To receive body traits and genetic makeup as a result of genetic transmission is inheritance
- Variation that influence gene function are usually referred to as mutation.
- Variation not affecting health is polymorphism (an allelic variation within a species).
- Mutation can take place in Somatic and Germ cells.
Unifactorial Inheritance
Defect in a single gene.
Follows Mendelian’s law.
Types:
- Autosomal Dominant and Recessive
- Sex linked Dominant and Recessive
Autosomal dominant inheritance:
- Inheritance of dominant gene on autosome
- Appears in each generation.
- Male and female offspring are equally affected (not influenced by sex).
- Dominant trait is manifested in Heterozygote.
- Normal and abnormal genes (alleles) are present.
- One mutant gene is sufficient to produce the character.
- An affected parent is always present or is due to new mutation. Unaffected person do not transmit the trait.
- Severe case is either infertile or die on childhood.
- Severity is variable. The variability is referred to as expressivity. In osteogenesis imperfecta the severity varies from blue sclera to blue sclera + deafness + multiple fractures+abnormal dentitions.
- Sometimes the mutant gene can’t produce effect, in such condition the gene is termed non-penetrant. The mutant gene is modified by other genes and environment.
- Example: Hutington’s disease, Neurofibromatosis
Autosomal recessive inheritance
- Both the genes on autosomes are affected.
- Low incidence.
- Recurrence risk: 1 in 4
- Both sexes are equally affected.
- Appear suddenly in the family.
- Consanguinity increases the rate of incidence.
- Affected offspring may or may not have an affected parent.
- Enzyme proteins are affected in many cases.
- In 4 children, 1 is normal; 2 are born with a normal and abnormal gene (carriers) and 1 with 2 abnormal genes (at risk for disease)
- Examples: Sickle cell anaemia, Beta-Thalassemia, Cystic fibrosis
Sex linked inheritance
- Genes are on sex chromosome.
- There are 2 functions of sex chromosomes: sex determination and control of some metabolic activities.
- In females, only 1 X chromosome remains active and other remains inactive and is seen as condensed dark body (Barr body)
Types :
Y-linked
- Only males are affected.
- Sons of affected male inherit the trait. e.g. Hairy ear
X-linked
- Defect in genes of X chromosome.
- Female can be heterozygous or homozygous for mutant gene.
- Absence of father to son transmission.
X-linked Dominant Disorders:
- abnormal gene dominates the gene pair
- Both sexes are affected.
- Males are severely affected.
- If father carries abnormal X gene, all daughters will inherit the disease and sons are normal.
- Affected heterozygous females transmit these disorders to male and female children equally; half of their children will inherit the disease tendency.
- Examples : Vitamin D-resistant rickets
X-Linked Recessive disorders:
- Males are mostly affected.
- Both matching genes be abnormal for disease
- Rarely in females e.g. Turner syndrome
- May skip a generation
- Trait may be transmitted through a series of female carriers
- Examples: Deuchenne muscular dystrophy, Hemophilia
Inborn Errors of Metabolism:
- Genetically determined biochemical disorder in which a specific enzyme defect causes a metabolism block
- Expressed only in homozygotes while heterozygotes are carriers
- Errors of amino acids, carbohydrate, lipid and mineral metabolism
- May be able to treat if diagnosed early
- Eg. : phenylketone-urea, albinism, mucoplysaccharidosis
Steps of Clinical Genetics:
- History Taking
- Pedigree charting(family tree)
- Clincal examination: urinogenital examination
- Dermatoglyphics:
- print of both hands and finger tips recorded with ink
- analysis of total ridge count and atd angle
- normal atd angle is 38 – 40 (increased in Down’s Syndrome and decreased in Klinefelter’s Syndrome)
- Buccal smear: Buccal mucosa smear examined for presence of barr body to detect genetic sex of person
- Karyotyping
- Biochemical assays
- Other investigations: X rays, biopsy, biochemical investigations
- Counselling
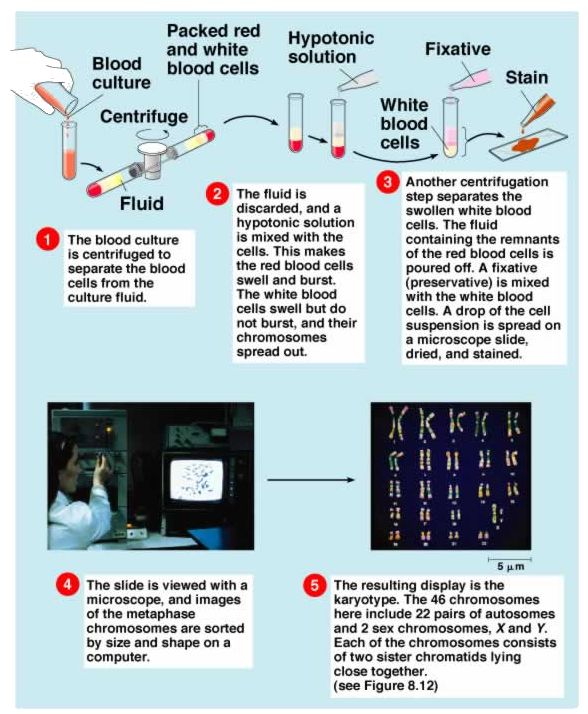
- Karyotyping is a method of study of chromosomes in which a set of chromosome arranged in a standard classification from photomicrograph of metaphase is studied.
- From peripheral blood lymphocytes, bone marrow, skin, amniotic fluid cells
Indications for chromosome analysis:
- Multiple congenital abnormalities.
- Unexplained mental retardation.
- Sexual ambiguity.
- Infertility.
- Recurrent miscarriage.
- Still birth.
- Malignancy & chromosome breakage syndrome
Method: routine blood cultures
- Blood planted in culture vials containing tissue culture medium supplemented by phytohemagglutinin (PHA)
- Commonly used media are TC199, HAM F10, RPM1, etc. having nutrients and human AB serum
- Heparin used as anticoagulant
- Antibiotic added to prevent contamination
- PHA in culture vials stimulate cell division
- Vials kept for incubation at 37 c
- At 69th hour, colchicine is added for cell division arrest
- After 1 – 3 hours, centrifugation, supernatant discarded and cells treated with hypotonic KCl solution allowing cells to swell
- Centrifugation again, supernatant discarded and fixative (methanol and acetic acid) added
- Slides prepared and observed microscopically
- Atleast 30 chromosome spreads analysed
Classification of Chromosome:
Chromosome consists of centromere and 2 arms labeled as p and q
Classification By Position of Centromere:
- Metacentric
- Submetacentric
- Acrocentric: Except Y chromosomes, all have satellites attached by secondary constricitions
- Telocentric
Denver Classification: arranged in decreasing size
- A: 1, 2, 3
- B: 4, 5
- C: 6 to 12, X
- D: 13, 14, 15
- E: 16, 17, 18
- F: 19, 20
- G: 21, 22, Y
1, 3, 16, 19, 20 (metacentric)
13, 14, 15 (large acrocentric with satellites)
21, 22 (small acrocentric with satellites)
Y (acrocentric without satellites)
Remaining submetacentric
Genetic Counselling
Steps of Genetic Counselling:
- Accurate diagnosis of disorder
- Advising the patient/ family members
- Management of disorder either curative/supportive
Prenatal Diagnosis:
Indications :
- Advanced maternal age
- One of the parents is a balanced translocation carrier.
- If autosomal or X-linked recessive metabolic disorder.
- One child with neural tube defect.
Procedure:
- Amniocentesis
- Chorionic villi sampling
- Ultrasonography
- Fetoscopy
- Fetal blood sampling
- Maternal blood sampling
- Preimplantation diagnosis
Amniocentesis:
- Amniocentesis involves aspiration of amniotic fluid for biochemical and/or genetic investigation.
- Optimum time- 16 to 18 weeks,2nd trimester.
- Cells obtained cultured for 1-3 weeks.
- Prepare the karyotype.
- Banding to determine the structural arrangement
Chorionic Villus Sampling:
- 9-12 weeks, during first trimester.
- USG evaluation of pregnancy is performed beforehand.
- Rather easy and less traumatic.
- Direct analysis of chromosome / 24 hrs. after culture
Ultrasonography:
- Done routinely for the verification of viability of embryo, determination of gestational age, diagnosis of multiple gestations, diagnosis of various congenital anomalies and well as guide for the passage of instruments for invasive procedures.
Fetoscopy:
- Visualization of fetus using a fiber optic self-illuminated instrument.
- Inserted in the amniotic cavity under local anesthesia.
- 18-22 weeks of gestation.
- Detect the limb malformation, facial defect, cleft lip, cleft palate, ear deformities.
- 3-5% abortion but useful for skin biopsy and fetal blood sampling.
Fetal and Maternal Blood Analysis:
- An attractive method because of its non- invasiveness nature.
- Fetal cells get available in the maternal blood after15 weeks of gestation.
- Difficulties in extraction of fetal cell.
- 20 ml sample may contain 0-20 fetal cells.
- 1fetal cell/ 1 million maternal cells.
- Need to be improvised to make it a standard procedure.
- Maternal blood can be used for assessment of neural-tube defect.
- Raise in the alpha-fetoprotein level in the serum of maternal blood.
Preimplantation Diagnosis:
- Suit for IVF procedure
- Fertilize ovum get developed into 8 celled stage.
- One of the cells taken out to assess genetic defect.
- If not found any disorders then get implanted into mother’s womb for pregnancy.
- Useful for those who can’t terminate the pregnancy due to religious background.
Chromosomal Abberation:
- Definition: Abnormalities of chromosome.
- Frequency: 6/1000 live birth
- Major cause of spontaneous abortion, congenital malformations, mental retardation and malignancies.
Classified as:
- Numerical
- Structural
- Different Cell lines
Numerical Chromosomal Abnormalities:
- Variation in Chromosomal number than normal.
- Classified as:
- Aneuploidy
- Euploidy or Polyploidy
Gain or loss of one or more chromosome.
Types:
- Trisomy: Extra homologous chromosome. Eg. Trisomy 21(Down syndrome), Trisomy 18, Trisomy 13
- Tetrasomy: Extra homologous pair.
- Monosomy: Absence a chromosome. Eg. Turner syndrome (45,XO)
Cause:
- Trisomy: Non-disjunction in M-I (75%) or M-II (25%).Mostly maternal in origin.
- Tetrasomy: Incomplete div in early cleavage
- Monosomy: Loss of the chromosome as it moves to the pole .
Examples: Trisomy 21, Trisomy 18, Trisomy 18, Klinefelter (47,XXY), Super female (47,XXX), Turner syndrome (45,XO)
Down’s Syndrome:
- Trisomy 21 mainly; translocation (4%); mosaicism (1%)
- Incidence of 1:800 live births
- High correlation between maternal age and meiotic non-disjunction
- Extra chromosome is small acrocentric 21
- Chromosome number 47
- Symptoms:
- Mental retardation (IQ<50)
- Small stature, Flat nose, malformed ears, epicanthal folds
- Constantly open mouth with protruding tongue
- Delayed dentition, septal defects, high incidence of leukemia
- White spots on the periphery of iris
- Generalized muscular hypotonia, round cranium
- Simian creases in about 50 % cases
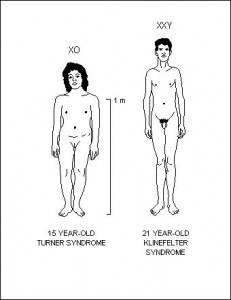
Turner Syndrome:
- Monosomy (45,X)
- Incidence of 1:3000 female births
- Symptoms:
- Short stature
- Webbing of neck
- Low hairline
- Cardiovascular abnormalities
- Small finger and nails
- Ovary poorly developed
- Secondary sexual characters like pubic hair, external genitalia, breast development weakly manifested.
- Nipples widely spaced
- Shield-shaped thorax
- No menstruation
- Elbow deformity
Klinefelter’s Syndrome:
- Trisomy (47,XXY)
- Incidence of 1:850 male births
- Rarely diagnosed before puberty
- Symptoms:
- Tall and thin stature
- Poorly developed secondary sexual male characteristics like beard, chest hair, pubic hair
- Narrow shoulders and wide hip
- Gynecomastia
- Reduced testicular size, scrotum and penis hyperplasia
Structural Chromosomal Abnormalities:
Alteration in chromosomal structure.
Causes:
- Reconstitution in unusual combination following chromosomal breakage.
- Improperly lining up of chromosome during meiosis.
- Exposure to teratogen.
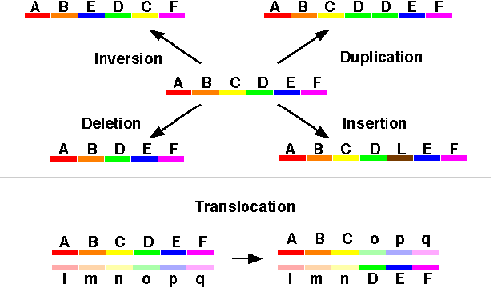
- Further classified as:
- Deletion: A portion of the chromosome is missing or deleted. eg. Wolf-Hirschhorn (deletion of 4p), Cri-du-chat (deletion of 5p), Prader-Willi syndrome (microdeletion of 15q), Angelmann syndrome (microdeletion of 15q)
- Duplication: A portion of the chromosome is duplicated, resulting in extra genetic material. eg. Charcot-Marie-Tooth disease type 1A (duplication of gene encoding PMP22 on chromosome 17.
- Ring Chromosome: A portion of a chromosome has broken off and formed a circle or ring.
- Isochromosome: Formed by the mirror image copy of a chromosome segment including the centromere.
- Translocation: When a portion of one chromosome is transferred to another chromosome. There are two main types of translocations.
- In a reciprocal translocation, segments from two different chromosomes have been exchanged.
- In a Robertsonian translocation, an entire chromosome has attached to another at the Centromere – in humans these only occur with chromosomes 13, 14, 15, 21 and 22.
- Inversion: A portion of the chromosome has broken off, turned upside down and reattached, therefore the genetic material is inverted.

Cri-du-chat Syndrome:
- Chromosome 5p deletion syndrome
- Incidence: 1 in 50,000 live births (male : female ratio of 3 : 4)
- Symptoms:
- Cat like cry during infancy
- Microcephaly
- Anti-mangoloid slant of the palpebral fissure
- severe cognitive, speech, and motor delays.
- behavioral problems such as hyperactivity, aggression, tantrums, and repetitive movements.