Understanding Lupus: Evaluation and Management
In the previous article, we tried to understand how SLE patients present and when to suspect it. Most of the time, the disease just keeps glaring at us and we still miss it because we do not think about it. Now once we have suspected SLE on the basis of clinical symptoms and confirmed it my serological tests, we need to decide how aggressive do we need to treat that particular patient. This depends on whether the patient has ‘life threatening’ or ‘non-life threatening’ disease (refer to previous article).
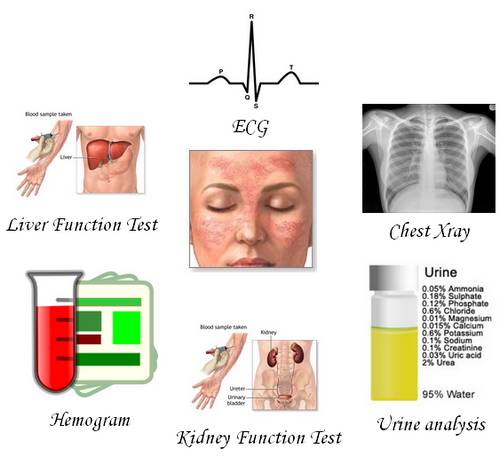
Investigations to be done for all lupus patients (both groups):
- Complete hemogram
- Kidney function test
- Liver function test
- Chest xray
- ECG
- Urine routine examination
- 24 hour urine albumin or urinary albumin: creatinine ratio
- Urine for active sediments (ie dysmorphic RBCs, RBC and WBC casts)
- Urine RBC morphology
The last three investigations are done if urine routine examination reveals more than trace proteinuria or hematuria. The investigations are primarily indicated to identify any subclinical organ involvment.
Investigations done in life threatening cases (in addition to above):
- dsDNA titres
- C3 and C4 levels
- APS panel including anti-cardiolipin Ab (IgM and IgG), Lupus anti-coagulant and beta-2 glycoprotein-1 levels (espcially if anti-phospholipid syndrome is suspected)
- Cultures from possible infected sites (Blood, urine, sputum, pleural fluid etc) if sepsis is a possibility. Most cases of lupus patient having sudden deterioration in their clinical condition are likely to have infective etiology (as a complication of immunosuppressive treatment)
- HRCT chest or PFT with DLCO ( in acute presentation of ILD or alveolitis)
- Bone marrow examination, coombs test , reticulocyte count in cases of cytopenias.
TREATMENT:
A) NON LIFE THREATENING:
This basically includes SLE diagnosed on the basis of joint and muco-cutaneous complaints. The subclinical renal involvement needs to be ruled out before labeling the patient as having non-life threatening disease. Treatment of this category will include:
- Low dose prednisolone. May be started at 0.5mg/kg and gradually tapered over 3months.
- Hydroxychloroquine sulfate 200mg twice daily
- Non-steroidal anti-inflammatory drugs: for temporary control of pain and inflammation on as required basis only.
- Sunscreen application with SPF >= 30 for skin rashes and photosensitivity.
- Mild cutaneous involvement only may be managed by low potency topical steroids by dermatologists.
Some patients with mild cytopenias or refractory synovitis and those who are unable to taper steroids may require addition of immunosuppressant like azathioprine (1-2mg/kg/day) or cyclosporin (2-3mg/kg/day in divided doses)
B) LIFE THREATENING:
This is a condition when you need to treat the patient aggressively. Usually these patients require workup and treatment simultaneously. After confirmation of lupus as the etiology for patient’s condition (be it rapidly progressing renal failure, worsening dyspnea, mesenteric ischemia, refractory or recurrent seizures) or if these manifestations are seen in a patient previously diagnosed as lupus (may be as non life threatening initially), then aggressive immnunosuppression needs to be instituited.
Intravenous methylprednisolone 1gm daily for 3 doses is the most rapid acting drug. This however needs to be followed by cyclophosphamide or rituximab as a definitive treatment. If you cannot rule out co-existing infection then it is always safe and pragmatic to put the patient on broad spectrum antibiotic coverage according to local sensitivity pattern.
Once the condition of the patient is stabilized, they should be maintained for a long time on immunosuppressant and be monitored regularly.
COMMON PRACTICAL ERRORS SEEN IN CLINICAL PRACTICE:
I was not sure whether I should write in this heading but then I thought the whole purpose is to clean up the mistakes we are doing by sharing them amongst us. So here are few of them:
1) Waiting for renal biopsy report before starting high dose steroids in patients with RPRF (rapidly progressive renal failure). If you have adequate evidence that the disease is lupus, eg by compatible clinical picture and positive ANA and high titres DNA, then you should not wait to document the renal histology before saving the patient. An early administration of high dose steroids can be kidney and life saving in such situations. If you wait for creatinine and patient to stabilize before a biopsy then a diagnosis may be only documented at autopsy or little less the patient may land up with shrunken kidneys and dialysis for lifetime!
2) Starting cyclophosphamide but not methylprednisolone: This again is seen quite commonly and the logic is ‘avoiding steroids’. Wow! We better save the organ first than think of osteoporosis years later. And, it is not the high dose given for few days that matter but the long toxic doses given cause all the harm. Also, it should be remembered that intravenous cyclophosphamide takes at least 15days to act and that is enough time for the disease to destroy the kidneys. Steroids given in pulse acts within 48hours to save it!
3) Give options: There are other treatment options that are less toxic but extremely expensive. For example, rituximab, mycophenolate mofetil etc. Patients should be allowed to make an informed rational choice and we should not force them with our decision.

4) You do not need to repeat ANA titres to monitor the disease. If really needed one may use dsDNA and C3 levels to monitor impending flare or renal activity. Most of the times, clinical features and ESR/CRP are adequate for managing them.
Once these patients are stabilized, they need maintenance immunosuppression adequate to control the baseline activity. They should be frequently monitored to look for both the toxicity of medicines as well as early evidence of disease flare.




2 Comments
Nice article doc,
” We better save the organ first than think of osteoporosis years later. ” the phrase was catchy.
The Common mistakes segment was very helpful.
Keep it up.
Dear Dr Benetha,
Thank you for the comment. I hope there would be some change in practice of people who see this disease. Will try to update on other topics too.
Regards,
Binit
Comments are closed.