Understanding Hypothyroidism
Thyroid Hormones
The major thyroid hormones are T0-T2 and T3-T4.
T0 through T2 are considered inert hormones. They appear to be byproducts of thyroid hormone synthesis and do not appear to have any function in the body.
T3 and T4 are the hormones associated with hypothyroidism, and they play a crucial role in your metabolism. T3 is the primary hormone used to fuel your metabolism. T4 is a storage hormone that your body uses to make T3 as needed.
Hypothyroidism, a prevalent medical concern, is marked by the thyroid gland’s diminished ability to produce adequate thyroid hormones for optimal functioning, leading to a myriad of health complications. This condition is concerning due to the gland’s central role in regulating metabolism.
Iodine deficient Hypothyroidism
The thyroid gland uses iodine to make T3 and T4. Iodine deficiency is fairly rare in the United States because we put iodine in our table salt. You can also find iodine from dietary sources like sea vegetables, yogurt, fish and shellfish.
Those who do not use iodized salt, or have a very limited diet, are at risk for developing iodine deficient hypothyroidism.
The most common symptom of iodine deficiency is enlargement of the thyroid gland, also known as a goiter. If the condition continues, you could also experience the symptoms of hypothyroidism, including fatigue, weight gain and depression.
If you suspect you have an iodine deficiency, altering your diet could improve your iodine levels. T
If altering your diet and taking supplements does not relieve your symptoms within 30 days, consult your physician for further testing and diagnosis.
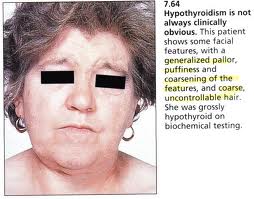
Autoimmune Thyroid Disease
Autoimmune thyroid disease, also known as Hashimoto’s thyroiditis, is the most common form of hypothyroidism in the US. The disease is caused by the immune system attacking the thyroid gland, which damages the gland causing it to malfunction. Unlike iodine deficient hypothyroidism, Hashimoto’s does not respond well to iodine. In fact, iodine makes the condition worse because it triggers the immune system to attack the thyroid.
The symptoms of Hashimoto’s include the symptoms of hypothyroidism – fatige, weight gain, depression, and sensitivity to cold. Individuals with Hashimoto’s can also have symptoms of other autoimmune diseases, like Gullian Barre, rheumatoid arthritis, or lupus. This is because a person with one autoimmune disease is at greater risk of developing other autoimmune diseases. Hashimoto’s disease, a common cause of thyroid problems, is typically identified through blood tests that detect increased levels of thyroid-stimulating hormone (TSH) and antibodies against thyroid peroxidase, an enzyme crucial for thyroid hormone production.
The disease can also affect children, although less commonly than adults. It can lead to slowed growth, delayed puberty, and poor school performance due to reduced mental function in children. Early diagnosis and appropriate management are crucial to mitigate potential impacts on a child’s development and overall well-being. Many online resources provide valuable insights into understanding and managing this condition, emphasizing the importance of regular medical check-ups and a comprehensive, personalized care approach.
The most common treatment for Hashimoto’s is thyroid hormone replacement using synthetic T4, also known as levothyroxine or Synthroid. Some physicians might supplement with synthetic T3, or with natural desiccated thyroid.
If you suspect you might have Hashimoto’s do not try to supplement with iodine or try to treat the condition yourself. Consult your physician for a thyroid antibody test to determine if you have the disease, then work with him to develop a treatment plan.
Radiation
Accidental exposure to enough radiation to destroy the thyroid is rare. Some prime examples are the survivors of the Chernobly disaster, who display higher rates of thyroid disease than comparable populations.
However, if a patient is suffering from an overactive thyroid, a doctor could prescribe radioactive iodine. The intent is to damage enough tissue to reduce the thyroid hormone output to normal levels. But administering radioactive iodine is not an exact science, and it is possible to damage too much tissue, making the patient hypothyroid.
For people with decreased thyroid function from radiation, iodine could help stimulate the remaining thyroid cells. But if too many cells are damaged, hormone supplementation could be the only course of action.They must take daily hormone replacement medication, typically a synthetic form of thyroxine (T4) known as levothyroxine, for the rest of their lives.
If you have received treatment for hyperthyroidism and suspect you might now be hypothyroid, consult your physician for testing.
With careful monitoring and appropriate medication, individuals who develop hypothyroidism after radioactive iodine treatment can effectively manage the condition and lead healthy lives. Regular follow-up with a healthcare provider is essential for optimal thyroid health management after RAI therapy.
Article by Jennifer Smith
Very aptly written…..
In fact hypothyroidism has become so common, especially among youngsters…..One should really move away from super dangerous junk food…….
They not only disrupt our eating habits but also deprive our body of the necessary nutrients…..
Nice article…….
Thanks for explaining in such detail……….