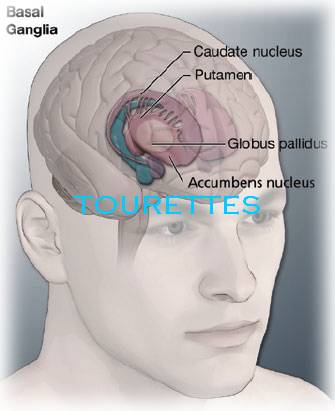
Tourette syndrome
“Tourette’s is just one big lifetime of tag, really. The world (or my brain-same thing) appoints me it, again and again. So I tag back. Can it do otherwise? If you’ve ever been it you know the answer.”
— Jonathan Lethem (Motherless Brooklyn)
Tourette syndrome (TS) is an iherited neurological disorder with onset in childhood, characterized by repetitive, stereotyped, involuntary movements (motor tics) and vocalizations (phonics or vocal tics); these tics characteristically wax and wane. People with TS have normal life expectancy and intelligence. Once considered as a rare disorder, TS is no more regarded as a rare disorder. Although TS can be a chronic condition, most people with the condition experience their worst symptoms in their early teens, with improvement occurring in the late teens and continuing into adulthood.
Other names:
- Tourette’s syndrome
- Tourette’s disorder
- Gilles de la Tourette’s Syndrome (GTS)
- Tourette’s
Onset: mostly between 7-10 years; generally before 21 years
Epidemiology:
- It is 3-4 times more frequent among males than among females
- Affects all ethnic groups, races in all parts of the world
Cause:
Tics are believed to result from abnormalities in cortical and subcortical regions, the thalamus, basal ganglia and frontal cortex of brain and the neurotransmitters like dopamine, serotonin, and norepinephrine that are responsible for communication among neurons.
a. Genetic factors:
- A person with TS has about a 50% chance of passing the gene to one of his/her children
- Not everyone who inherits the genetic vulnerability will show symptoms
b. Environmental, infectious, psychosocial factors:
- While not causing TS, can influence its severity
- Autoimmune processes may affect tic onset and exacerbation in some cases
Symptoms:
- Repeated involuntary movements
- Uncontrollable vocal sounds
- Facial tics
- Eye blinking
- Head jerking
- Neck stretching
- Foot stamping
- Throat clearing
- Coughing and sniffing
- Grunting
- Yelping
- Barking and shouting
- Lip biting
- Cheek biting
- Head banging
- Coprolalia (uttering swear words)
- Echolalia (repeating the words or phrases of others)
- Copropraxia (involuntary and affectively inappropriate use of obscene gestures)
- Echopraxia (involuntary imitation of the actions of others)
- Palilalia (involuntary repetition of parts of the individual’s own speech)
- Self-mutilation
- Facial grimacing
- Involuntary arm flapping
- Involuntary jumping, kicking, hopping, spanning
Tics are often worse with excitement or anxiety and better during calm, focused activities. Certain physical experiences can trigger or worsen tics, for example tight collars may trigger neck tics, or hearing another person sniff or throat-clear may trigger similar sounds. Tics do not go away during sleep but are often significantly diminished.
Complications:
- Deliberate self harm
- Choreoathetosis
- Self inflicted injury
Diagnosis:
According to the DSM-IV-TR, TS may be diagnosed when a person exhibits both multiple motor and one or more vocal tics over 1 year, with no more than 3 consecutive tic-free months.
These tests may also be required:
- MRI
- CT scan
- EEG
- Blood tests
Treatments:
- Some cases improve over time
- Neuroleptic drugs : risperidone, ziprasidons, haloperidol, pimozide, fluphenazine
- Sedatives
- Antihypertensive drugs : clonidine, guanfacine
- Tranquillizers
- Antipsychotic drugs
- Stress reduction
- Relaxation techniques
- Biofeedback
- Family counselling and psychotherapy to get rid of social stigma
The drugs may have severe adverse effects and patients have low compliance with the treatment
Sources:
Various magazines
Healthscout
Wrong diagnosis
Wikipedia