Rabies : Facts, Features and management Guidelines
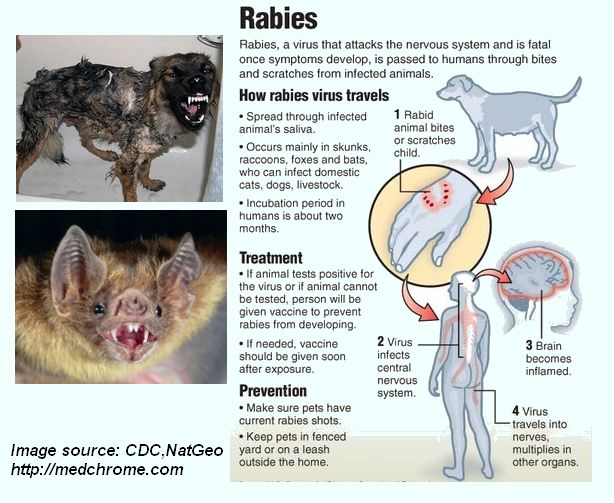
Rabies
Rabies is a zoonotic disease of warm-blooded animals is caused by a Rhabdovirus belonging to Lyssavirus. It is a bullet-shaped virus.
Mode of transmission-
Bites and licks on abrasions or intact mucus membrane by infected animals. Saliva is the vehicle of transmission. Bites, Licks, corneal graft, salivary aerosol can cause transmission.
Common sources of infection-
Rabid dogs, Monkey, Cat, Mice, Vampire bats.
Worldwide- Dogs, cats, canines, cattles, even Humans. Skunks, raccoons, vampire bats, cave dwelling bats in North and Latin America. For any wildlife spotted in your area, you can search for services like dead animal pickup to prevent some kind of infection or even disease.
Inoculation period – 9 days to months . In general its 4-8 weeks.
CNS and Salivary glands are the target organs of rabies virus. They travel from axons to the Brain.
Stages
I. Prodormal stage 1-10 days
II. Acute Neurological phase
III. Coma/Death
Clinical Features-
Not all people bitten by a rabid animal develop disease, but once it manifests it is almost always fatal.
- Fever
- Parasthesia at the bitten site.
- Anxiety
- Hydrophobia-50%, Photophobia, Aerophobia
- Delusion and Hallucinations
- Spitting, Biting, Mania
- Neurological abnormalities- descending paralysis
- Hyperpyrexia
- Death within a week.
On Examination-
- High fever
- Exaggerated jerks
- Spasticity
- Sympathetic overactivity- dilation of pupil
- Cause of death- Respiratory paralysis, cardiac arrhythmias.
Diagnosis-
History of bite, Examination of wound.
Immunofluroscent Study- Fluroscent Ab used to detect Ag. In Corneal impression and salivary secretion.
Classic Negri bodies detected in brain in Post-mortem examination. (99% cases). Negri bodies are eosionophilic cytoplasmic ovoid bodies 2-10 mm in diameter. Seenusually in cells of hippocampus and cerebellum.
Treatment-
Only symptomatic. Once the disease has started death is almost inevitable.
Patient should be kept in quite, dark room avoiding any stimuli.
Respiratory and Cardiovascular support may be necessary.
Nutritional Support.
Drugs- Morphine,Diazepam, Cholorpromazine.
All patient should receive post-exposure prophylaxis.
Tetanus toxoids and Antibiotics.
Care of wound after Bite by Animal-
- Immediately wash the wound with soap water for 5 minutes.
- Adequate cleansing of the wound.
- Virucidal agents- Alcohol, Tincture Iodine,Povidine Iodine can be used for cleaning.
- Do not suture the wound immediately, remove any necrotic debris if present.
- Tetanus toxoid.
- Watch for the symptoms in animal if traceable.
- Go for post-exposure Prophylaxis.
Guidelines for Post-exposure Prophylaxis.
- Category I- touching or feeding of animals, licks on intact skin
- Category II- Nibbling of uncovered skin, minor scratches,licks on broken skin.
- Category III- Single or multiple transdermal bites or scratches, contamination of mucus membrane with saliva.
Management-
- Category I- nothing needed
- Category II- Vaccine immediately.local treatment of the wound
- Category III- Rabies Ig + Vaccine immediately.local treatment of the wound
Vaccine- Human Diploid Cell-culture vaccine 1.0ml IM total 5 doses on 0,3,5,7,14,21 days.
Human Rabies Immunoglobulin- HRIg- 20 IU/kg ½ dose IM and other ½ injected around the wound.
Pre-exposure Prophylaxis-
Indicated for-
- Lab workers.

- Animal handlers.
- Vetenarians.
2 doses of HDCV 1.0ml deep Subcutaneous or IM. Re-enforcing dose after 12 months and then after every 1-3 years.
SOME FACTS on RABIES by WHO ( September 2010)
- Rabies affects more than 150 countries worldwide.
- Worldwide, > 55 000 die of rabies each yr.
- Dogs are the source of 99% of the rabies related deaths in Human.
- Wound cleansing and immunization within a few hours of contact can prevent the onset of rabies and death.
- Every year, more than 15 million people worldwide receive a post-exposure preventive regimen to avert the disease – this is estimated to prevent 327 000 rabies deaths annually.
Rabies Vaccines from CDC https://www.cdc.gov/vaccines/vpd/rabies/index.html