Alcoholic Liver Disease or ALD
Alcohol is a toxic substance to the liver and remains one of the most common causes of chronic liver disease..
The spectrum of ALD is broad and a single patient may be affected by more than one of the following conditions;fatty liver, alcoholic hepatitis or alcoholic cirrhosis.
EPIDEMIOLOGY

- ALD does not occur below a threshold of 21 units/week in women and 28 units/week in men. One unit is equal to 8g of alcohol , one glass of wine (125ml) or one 240ml can of 3.5-4% of beer. The average alcohol consumption of an individual with cirrhosis is 160g/day for an average of 8 years. Approx. 30-40 units of alcohol per week can induce cirrhosis in 3%-8% of individuals over 12 years.Fatty liver is the most commonly observed abnormality and occurs in upto 90% of alcoholics.
- Alcoholic cirrhosis is a common cause of ESLD , cirrhosis and hepatocellular carcinoma.
AETIOLOGY
- Acetaldehyde: 80% of alcohol is metabolised to acetaldehyde by enzyme alcohol dehydrogenase. Acetaldehyde forms adducts with cellular proteins in hepatocytes which activate the immune system leading to cell injury.
- 20% of alcohol is metabolised by the mixed function oxidase enzymes of the smooth endoplasmic reticulum. Cytochrome CYP2E1 is induced by alcohol, which increases oxygen consumption and lipid peroxidation. Microsomal peroxidation leads to oxygen free radicals which can induce mitochondrial damage.
- Cytokines: increased endotoxin is released into blood in alcoholic hepatitis via increased gut permeability. TNF-? production is increased from monocytes . release of IL-1,2 and 8 also occurs. These cytokines are also involved in fibrogenesis.
PATHOGENESIS
Cirrhosis develops when there is chronic and severe inflammation of the liver for an extended period of time. The regenerative capacity of the liver is enormous however over a long time fibrosis develops.
And when at least 70-80% of liver function has been lost the synthetic capacity of the liver is diminished.
PATHOLOGICAL FEATURES OF ALCOHOLIC LIVER DISEASE
- Alcoholic hepatitis: lipogranuloma
- Neutrophil infiltration
- Mallory’s hyaline
- Pericellular fibrosis
- Macrovesicular steatosis
- Fibrosis and cirrhosis
- Central hyaline sclerosis
CLINICAL FEATURES
Alcohol is a toxic substance to the liver and remains one of the most common causes of chronic liver disease.
The spectrum of ALD is broad and a single patient may be affected by more than one of the following conditions;
fatty liver, alcoholic hepatitis or alcoholic cirrhosis.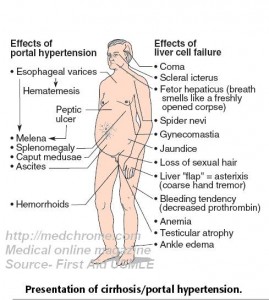
FATTY LIVER
-usually asymptomatic , hepatomegaly and mild liver enzyme abnormalities.
-fatty liver may be reversible with abstinence.
ALCOHOLIC HEPATITIS
-fever , upper abdominal pain , anorexia , nausea, vomiting, weight loss and jaundice.
-hepatomegaly and in severe cases features of portal hypertension (ascites , encephalopathy and gastrointestinal bleeding).
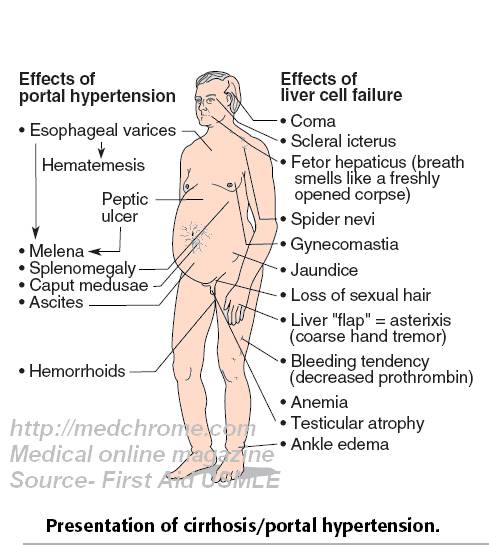
CIRRHOSIS
-large, normal or small liver
-ascites, varices, encephalopathy
-hepatocellular carcinoma
-stigmata of chronic liver disease:
Jaundice, spider telangiectasis, palmar erythema, cyanosis, parotid swelling, Dupuytren’s contracture, loss of libido , hair loss, gynaecomastia , testicular atrophy, impotence , breast atrophy , irregular menses, amenorrhoea , bruises, purpura , epistaxis , menorrhagia , splenomegaly, collateral vessels, variceal bleeding, hepatic encephalopathy, digital clubbing.
INVESTIGATION
- Macrocytosis in the absence of anemia may suggest and support history of alcohol misuse.
- In alcoholic fatty liver mild elevation in serum aminotransferases (AST higher than ALT ratio AST:ALT>2) and ALP.
- In alcoholic hepatitis elevation in serum aminotransferases(AST higher than ALT) and ALP.
- Hyperbilirubinemia, prolongation of PT ,lactic acidosis, hyperuricemia , elevated TGL , thrombocytopenia ketoacidosis, hypoglycaemia , cdt>20u/l , raised GGT.
- Laboratory abnormalities with poor prognosis include renal failure, leukocytosis, a markedly elevated total bilirubin and prolongation of PT that do not normalise with vitamin K.
- A Discriminant function(DF) or Maddrey’s score enables to assess prognosis in alcoholic hepatitis.
- DF=4.6-[PT patient – PT control]+serum bilirubin(mg/dl)
- A value over 32 implies severe liver disease with a poor prognosis.
TREATMENT
Behavioural cessation of alcohol is the single most important treatment. Abstinence is even effective.
Good Nutrition is very important and enteral feeding via a fine-bore nasogastric tube may be needed in severely ill patients.
-Patients with DF>32 and hepatic encephalopathy may benefit from steroid therapy. Oral prednisone can be started at 40-60mg/day and subsequently tapered.
Pentoxifylline 400mg PO tid is a nonselective phosphodiesterase inhibitor with anti-inflammatory properties ; reduce incidence of hepatorenal failure and has shown improved survival in severe alcoholic hepatitis.
S-adenosylmethionine, antioxidants , tumor necrosis factor inhibitors are under investigation in ALD.
Greetings I just now finished reading your web blog and I’m very impressed. I actually do have a few questions for you though. Are you currently intending on doing a follow-up article about this? Do you think you’re likely to keep posting as well?