Alcohol Related Disorders
Alcohol are hydroxy derivatives of aliphatic hydrocarbons.
Manufacture:
C6H12 O6 (sugar) ----zymase----> 2 CO2+ 2C 2 H 5 OH
Metabolism of Alcohol:
- Alcohol is metabolized in liver by alcohol dehydrogenase
- 90% – processed in liver
- 10% – excreted (eliminated unchanged from kidneys and lungs)
- Absorption mostly from small intestine and only 10% from stomach.
- Peak effect in 30 to 90 min (30 to 60 min in empty stomach)
- Depends upon:
- time of food intake
- duration of consumption
- type of drink consumed
Alcohol—(1)—>acetaldehyde—(2)—>acetic acid —>CO2+ H2O
- 1 = Alcohol dehydrogenase
- 2 = Aldehyde dehydrogenase
Concentration of Alcohol in Different Liquors:
- Beer : 4 – 8%
- Wine : 12 %
- Whisky and other liquors: 40%
- Illicit: 20 – 40 %
- 1 unit = 30 ml of whisky or 360 ml of beer or 120 ml of wine
- In 70 kg person 1 unit gives 15 – 20 mg/ dl of blood level
- Safe drinking: Men (21 unit/ week) and Women (14 unit / week)
Caloric values of Alcohol
- Alcohol is full of calories

- 2 – 3 gin and tonic/day for 4 wks will increase wt about 4 pounds.
- 1 pint of beer = 1000- 2000 kcal
Determinants of BAC (Blood Alcohol Content):
- Quantity/ speed of drinking.
- Concentration of alcohol in the drink.
- Body fat (W BAC 20 % > M)
- Addition of soda carbonated beverage.
- empty stomach.
- Body wt: higher the body wt lower the BAC.
- Carbohydrate food in stomach delays absorption.
BAC (mg/dl) vs Behavior (Correlation):
- < 80: Euphoria, feeling of relaxation, talking freely, reduced alertness
- >80: Noisy , moody , impaired judgment
- 100-200: Blurred vision , unsteady gate, gross motor incordination , slurred speech, aggressive, quarrelsome and talking loudly
- 200-300: Amnesia for experience( alcoholic blackout)
- 300-350: coma
- 350-600: death
Levels of Alcohol Use:
- Social use: without any apparent harm, exploration for curiosity, group activity, to relieve anxiety, dissolve inhibition, facilitate social interaction , dietary practice religious rituals.
- Harmful use/abuse: leads to impairment in one of more areas of daily life (physical , social , occupational , family life, legal involvement)
Alcohol dependence:
- Feeling of “compelled to drink”
- A stereotyped pattern of drinking
- Alcohol takes priority over anything else
- Development of tolerance
- Psychological and physical withdrawal symptoms
- Relief after drinking
3 or more of the following must have been experienced or exhibited at some time during the previous year:
1. Difficulties in controlling substance-taking behavior in terms of its onset, termination, or levels of use
2. A strong desire or sense of compulsion to take the substance
3. Progressive neglect of alternative pleasures or interests because of psychoactive substance use, increased amount of time necessary to obtain or take the substance or to recover from its effects
4. Persisting with substance use despite clear evidence of overtly harmful consequences, depressive mood states consequent to heavy use, or drug related impairment of cognitive functioning
5. Evidence of tolerance, such that increased doses of the psychoactive substance are required in order to achieve effects originally produced by lower doses
6. A physiological withdrawal state when substance use has ceased or been reduced, as evidence by: the characteristic withdrawal syndrome for the substance; or use of the same (or a closely related) substance with the intention of relieving or avoiding withdrawal symptoms.
CAGE QUESTIONNAIRE FOR DIAGNOSIS OF ALCOHOLICS
- C- Have you ever tried to Cut down on alcohol (amount)?
- A- Have you ever been Annoyed by people’s criticism of alcoholism?
- G- Have you ever felt Guilty about drinking?
- E- Have you ever needed an Eye opener drink (early morning drink)?
A score of 2 or > identifies problem drinker
Clinical Features:
- Neglect of other activities.(social, occupational , recreational)
- Excessive use:- consumed in large amount over a long period of time.
- Impaired control of drinking habit.
- Persistence of use in-spite of physical or psychological problem created by it.
- Large amount of time spent in alcohol related activities.
- Withdrawal symptoms:- N/V, shaking, sweating, anxiety
- Tolerance:- need of increasing amount of alcohol to feel its effect.
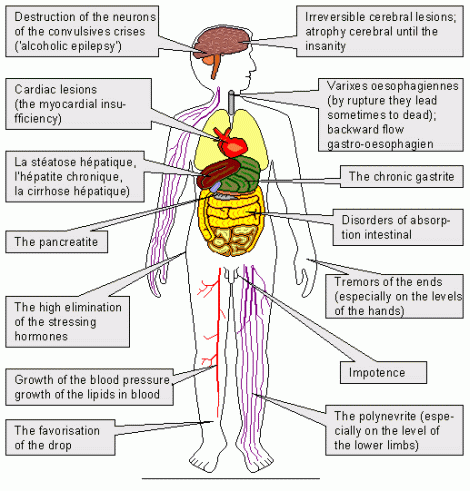
COMPLICATIONS
A) Medical complications
- Gastrointestinal: gastritis, reflux oesophagitis, esophageal avarices, peptic ulcer, ca stomach and stomach, malabsorption syndrome, pancreatitis
- Hepatic: fatty liver, cirrhosis of liver, hepatitis, carcinoma liver.
- CNS: peripheral neuropathy, delirium tremens , rum fits, alcoholic hallucinosis , wernicke- korsakoff psychosis, alcoholic dementia, cerebellar degeneration, alcoholic myopathy, suicide
- CVS: Cardiomyopathy, hypertension.
- Hematological: anemia, leucopenia, decrease platelet and increase MCV
- Metabolic: ketoacidosis, hypoglycemia, hypocalcaemia, hypomagnesaemia
- Miscellaneous: Osteoporosis, psoriasis, fetal alcohol syndrome, impotence decrease immunity etc.
Accidents, marital disharmony, divorce, occupational problems,increase incidence of drug dependance, criminality, financial difficulties.
Acute alcohol intoxication
- Brief period of excitement then generalized CNS depression.
- Increased reaction time, slowed thinking, distractibility, and poor motor control.
- Later: dysarthria , ataxia and in coordination, progressive loss of self control.
Alcohol withdrawal syndrome
Abrupt cessation or rapid decrease in amount of alcohol consumption causes:
- Minor withdrawal symptoms (12 – 18 hrs):
- tremors
- nausea/ vomiting
- tachycardia
- HTN
- weakness
- anxiety
- insomnia
- Major withdrawal symptoms:
- Delirium tremens
- Alcoholic seizure (rum fits)
- Alcoholic hallucinosis
Delirium Tremens:
- Severe withdrawal syndrome, life threatening
- Starts 2- 3 days after cessation of alcohol intake and features last for 3 – 7 days.
- Acute organic brain syndrome with feature of :-
- Clouding of consciousness with Disorientation in time , place, person
- Poor attention span and distractibility.
- Visual , auditory hallucination, tactile hallucination, illusion , delirium.
- Autonomic disturbance:- tachycardia, sweating, fever, HTN, pupillary dilatation
- Psychomotor agitation, ataxia
- Insomnia
- Dehydration with electrolyte imbalance
Alcoholic Seizures (Rum Fits):
- Generalized tonic clonic seizures occur in about 10% of alcohol dependence ptn. After 12- 48 hrs after cessation or decrease in amount of alcohol.
- Multiple seizures (2-6 at one time) common than single seizures.
Alcoholic Hallucinosis:
- Usually auditory hallucination during partial or complete abstinence following regular alcohol intake.
- In 2% patients.
- Persists after the withdrawal syndrome is over and classically occurs in clear consciousness.
- Usually recovery occurs within one month and the duration is very rarely > 6 months.
Wernicke’s Encephalopathy:
- This is an acute reaction to severe def of thiamin.
- Imp clinical signs:-
- Ocular signs:- nystagmus, ophthalmoplegia,b/l external rectus paralysis, pupilary irregularities, retinal hemorrhages and papiloedema
- HMF disturbances:- disorientation, confusion, recent memory disturbances, poor attention span and distractibility, apathy and ataxia.
- Follows wernicke’s encephalopathy
- Together refered as wernicke’s korsakoff’s psychosis.
- Cause: severe, untreated thiamin deficiency secondary to chronic alcohol use.
- Clinically presents as organic amnestic syndrome characterized by gross memory impairement (anterograde amnesia) and confabulation.
Treatment:
A) Before treatment
- Rule out physical disorder, psychiatric disorder,
- Assessment of motivation for treatment.
- Assessment of social support system
- Assessment of personality characteristics of the patient
- Assessment of the current and past social interpersonal and occupational functioning.
B) Detoxification in hospital for 7 to 14 days:
- Benzodiazepines:
- Chlordiazepoxide (80 – 200 Mg/day in divided dose).
- Diazepam (40 – 80 Mg/day in divided dose)
- Carbamazepine (600 -1600 Mg/ day)
- I.v. Thiamine 100 mg bid for 3 – 5 days followed by oral admin of B1 for at least 6 month.
- Good nutrition with vitamin B,C, A supplements.
Treatment of Alcohol Dependence:
Psychotherapy
Deterrent agents: Disulfiram 250- 500mg/day at bedtimes for 1 wk, then 250 mg/ day maintenance dose
Anti-craving agents
- Acamprosate
- Naltrexone
- Fluoxetine
- Others: benzodiazepines, antidepressants, antipsychotics, lithium, carbamazepine, narcotics for special use.
Psychosocial rehabilitation
Treatment of Withdrawal Syndromes:
- Minor withdrawal: chlordiazepoxide or oxazepam
- Delirium Tremens: iv benzodiazepines and supportive care nutrition, electrolyte balance, vit B complex.
- Alcoholic seizures: iv benzodiazepines
- Alcoholic hallucinosis: neuroleptics ( haloperidol 2 – 5 mg bid)
- Wernickes encephalopathy: thiamine (100 mg IM)






3 Comments
Alcohol is capable of causing birth defects. Colon cleanser help build strong immune to fight disease that develop from alcohol, This capability classifies it medically as a teratogen. Alcohol is now recognized as the leading teratogen to which the fetus is likely to be exposed. This applies only to societies in which alcoholic beverages are consumed. In these populations, prenatal alcohol exposure is thought to be the most common cause of mental retardation.
thank you for reading my article…
yes you can use it for presentation and even modify it in your presentation.but please do not publish in any other site
Can this be used by readers for presentations? can I modify it. is it copy righted?
Comments are closed.