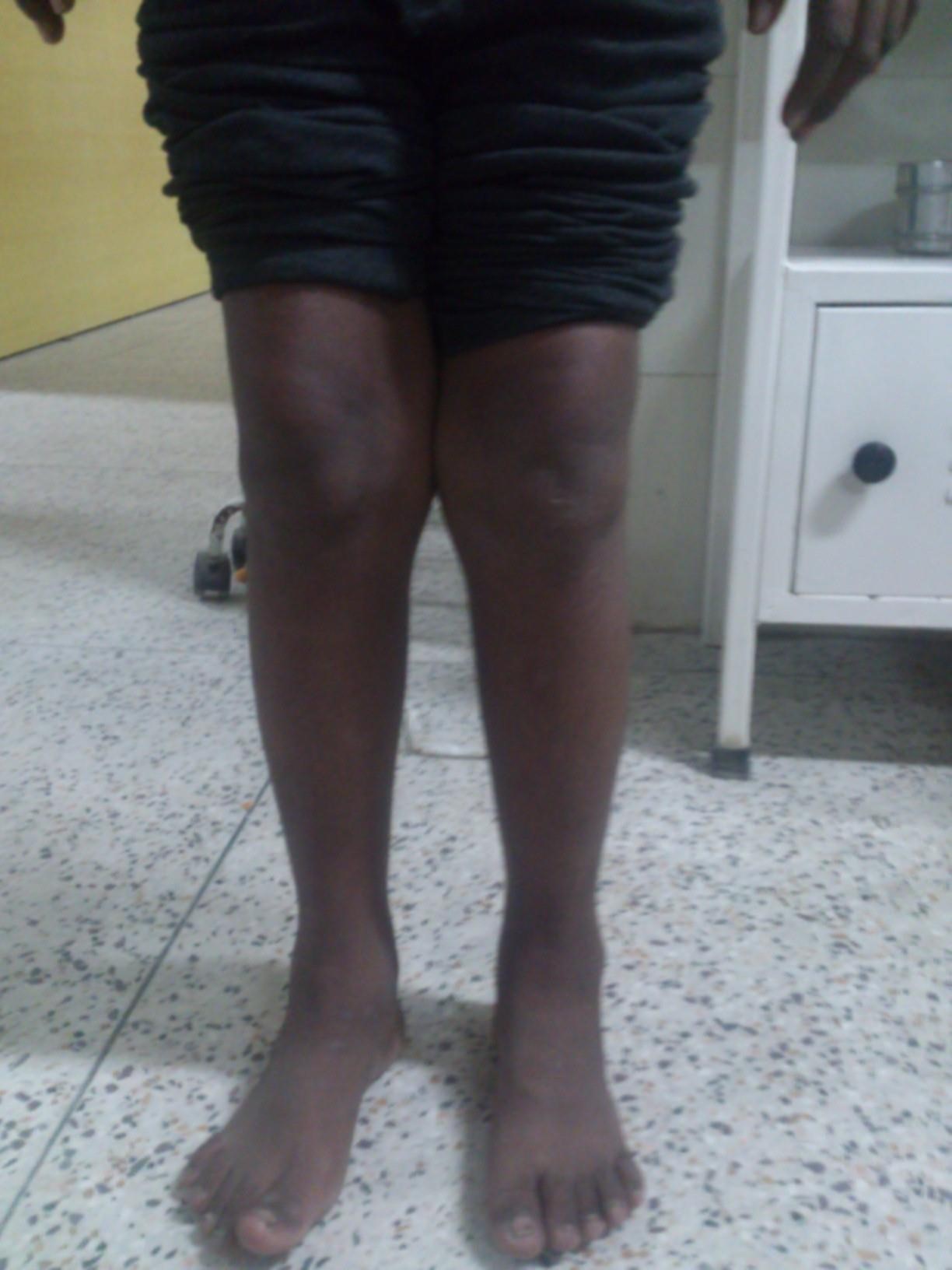
Wilson disease presenting with Cirrhosis and Refractory Rickets
A 11 yrs Male presented with complains of Difficulty in walking for 4 months, Deformity of legs noticed for same duration and Diffuse muscle and bone pains.
Child was well before 4 months
1. Started complaining of limb pain, Onset gradual and slowly progressive, -diffuse, ill-localised pain in limbs & joints, Mild to moderate severity, missed school, -unable to walk steadily and for long distance and child had swaying and limping during walking,Had to sit after walking due to weakness and fatigue, Child is not able to lift glass steadily, Trembling +
2. Joint deformity+ for same duration, gradually, increased widening of the wrist, knee and ankle joints, No swelling, pain, redness or limitations of movements, Generalized bodyache+
No localized bone or muscle pains, No associated fever, rash, photophobia, redness of eyes, or morning stiffness.
No genital or oral ulcerations.Has h/o reddish urine on/off , 1 episode was associated, with fever received treatment but has episodes +,on/off
Burning + on/off, straining -, urgency-, frequency- Frothy urine-, excessive amount of urine –
• No h/o fall, no SOB, palpitations, cough, swelling of body
• No h/o tingling sensation or numbness, burning sensation over limbs, No h/o incontinence, or retention of urine, constipation+
• Facial deviation-, double vision-, eye deviation-, dysphagia -, Hoarseness of voice -, change in voice –
• No diurnal variation of weakness, no lid falling, no slipping of slippers, difficulty wearing clothes buttoning, able to lift hand over the head
• No h/o jaundice in the past, no h/o fat indigestion, passing bulky stool, recurrent diarrhea or frothy stool
• Rashes-, bleeding manifestations -, no h/o progressive, pallor, lumps over neck and axilla
• Headache + on/off ,vomiting -, LOC -, abnormal movements –
• No polydipsia, increase urine
• No long term use of any medication before onset of illness
• No h/o abnormal body movements, change in behavior
Family history
No h/o renal disease, bony deformity or malformations, or liver disease
• Consanguinity + 2nd Degree
• No h/o fetal wastage, No h/o neonatal deaths
• No short stature in family members
Developmentally normal for age
Nutritional-
Intake of calorie was adequate ( ~1800Kcal/day), non-vegetarian, consumes meat/fish 2 times/week
Adequate sun exposure ( plays outdoor games)
Examination-
• GC- fair, built – normal, no dysmorphism
Anthropometry-
OFC-51 cm , Ht-149 cm ( 50th Centile), wt-39 kg
( Normal)
Pallor +,Icterus -,Edema-,Lymph-,Dehydration – clubbing-
Skin- dry, Phrynoderma +; no scaling
Musculoskeletal examination
• B/L Genu Valgum +
• B/L Widening of knee joint and wrist
• No swelling, redness, tenderness
• No limitation of joint movement
• Muscles- non-tender, +
• Gait- waddling gait
• Stigmata of Rickets- Harrison sulcus-, costochondral beading-, kypho-scoliosis -, bossing of skull –
Other Systemic examninations
Chest/CVS- Normal
P/A- soft, liver + 3 cm. Span: 11cm, Spleen tip palpable +, BS +
CNS- HMF- Intact, cranial nerves and motor system
– Intact
No sensory symptoms, no cerebellar signs or
meningeal signs.
Hematological- no petechie,purpura,echhymosis, no bony tenderness.
Diagnosis
Provisional Diagnosis-
RICKETS
Differential Diagnosis
• Other Metabolic bone disease-
• Hypophosphatasia
• Metaphyseal Dysplasia
• Hyperphosphatesia
• Flurosis
Causes of Rickets
- Vitamin D Disorders
- Calcium deficiency
- Phosphorus deficiency
- Renal losses
Investigations
CBC- Hb- 11.5g/dl, WBC-normal Plateletes- N
Retic=0.6% PBS-normal
Urea/Creat= 3.3/83 mmol/L Na/K= 138/4.1
Work up for Rickets-
Ca-2 PO4- 3.5 ALP- 2943
LFT- Bil-normal alb-4.2 SGOT/SGPT- 36/121
Xray- Ankle,knee, wrist- Normal
Urine RME- WBC-2-4 RBC-plenty Alb 2+ Epi= 4-6
pH-5 Spg=1.015
iPTH- 22.3 pg/ml ( Ref- 7.5 to 53.5 pg/ml)
25-OH Vit D- 26.5 ( Insufficiency – 20-30)
USG done – nephrolithiasis, 4mm stone on rt upper pole
24 hr Ca/Cr ratio=1.07 (Hypercalciuria)
ABG- pH-7.45 pCO2-21.4 pO2-123 HCO3-15.6
Lac-2.5 anion gap –normal
TFT- Normal
Patient was treated for Vit D deficiency Rickets
• Received 6 Lac Unit of Vit D
• Discharged on Oral Calvit 1 tab BD for 4 weeks
Planned for F/U
Repeat USG done – B/L nephrolithiasis,
Liver- diffusely inhomogenous coarse echotexture.
On Repeat Admission
Repeat Evaluation-
• PT/INR-13,1.13
• SGOT/SGPT-46/27 ALP-2071
• Ca-2.2 P- 3.7
• Urine- RBC-10-12 RBC-plenty Oxalate-plenty
Sugar-nil Protein- trace
• Xray of wrist and knee- no improvement
Repeat USG done – B/L nephrolithiasis,
Liver- diffusely inhomogenous coarse echotexture, Portal vein calibre 13 mm.
Improvement?
Response is defined by radiological improvement within months, normalization of lab parameters, and improvement of bony defects
• Despite these therapeutic measures, there was little, if any improvement in his symptoms.
• X-ray- there was widening of metaphysis, with cupping and fraying, but typical finding of rickets was not seen.
Impresson- Refractory Rickets
DIFFERENTIATING
True rickets or rickets like states-
Preliminary investigations –
• Serum calcium, phosphate ,SAP
• X rays changes-
Rickets like (Metabolic bone ) disease –
– Hypophosphatasia
– Metaphyseal dysplasia
Is it just a Ricket-like states ?
1. Features – Radiological signs similar to rickets. But growth plate are not wide with differential involvement of bones in a joint. Eg. Femur shows changes but tibia is normal. Levels of serum Ca, P and SAP -normal. Diagnosis Metaphysial dysplasia.
2.Features -Clinical signs or rickets are present but x rays show tongue like radiolucency projecting from growth plate into metaphysis.SAP levels are low but S. ca, P Levels are normal.Diagnosis – Hypophasphatasia
In Our Case-
Ca, P- Normal
ALP- Raised ( >2000 )
Xray showed- rachitic changes
Impression – Rickets
Is it nutritional or non nutritional ?
Clues in the history or examination-
prematurity ,neonatal cholestasis ,anticonvulsant therapy , chronic renal diseaseà none were Present
Useful clues –
– Jaundice – hepatobiliary disease ,metabolic disorders
– Cataract – galactosemia, wilsons,
– Positive family history – metabolic disease, RTA
– Mental retardation, seizures – Galactosemia, drug induced rickets in primary CNS problem
– Alopecia – VDDR type 2
In Our Case-
No specific Clues – ?nutritional
Likely a non-nutritional cause?
Child received Vit D Therapy
– Non healing favors a non nutritional cause.
Features of non nutritional causes
– presentation before six months or after two years of age
– Associated failure to thrive
– Positive family history
– Obvious clues mentioned earlier
– Failure of vitamin D therapy
In our case- Trial with Vit D was given, after 1 month no clinical and radiological improvement
Non nutritional and lack any obvious clues – it could be either due to GI or renal cause
1. Features- Recurrent diarrhea, oily stools. Recurrent abdominal pain and distension. Anemia, hypoproteinemia. Multiple vitamin and mineral deficiencies. Diagonosis – Malabsorption with rickets.
2. Features –Hepatobiliary findings- Raised serum bilirubin, low serum, albumin and prolonged prothrombin time. Diagnosis – Hepatic rickets
3. Features- Failure to thrive, rec. vomiting, lethargy, acidotic breathing. Hypertension, anemia with or without edema. Positive findings in urine analysis. Abnormalities in electrolytes, blood urea and creatinine. Renal abnormalities in ultrasound abdomen. Diagnosis –Renal rickets.
Our patient had Hypercalciuria, Nephrolithiasis, urinary ptn+ and anemia.
Among Renal causes
Clinical features of chronic renal failure and on laboratory investigations- blood for electrolytes, urea and creatinine. blood gas analysis. ultrasonography of abdomen.
Features- Vomiting , lethargy, growth retardation, Hypertension, anemia, with or without edema, features of obstructive uropathy. Raised blood urea, creatinine. S. potassium may be high. Abnormalities in USG, MCU and DMSA scan. Diagnosis – Chronic renal failure – renal osteodystrophy.
Features -Recurrent vomiting, diarrhoea with acidotic breathing.Positive family history. Metabolic acidosis with normal anion gap, hypokalemia, and raised serum chloride. Normal blood urea and serum creatinine. No proteinuria or glycosuria. Diagnosis – Renal tubular acidosis.
Features- Severe form of rickets with stunting and deformity.Features mentioned in RTA. Proteinura, glycosuria present. Normal or slightly increased B.urea and S.creatinine. Features of underlying causes such as cystinosis. diagnosis. – Fanconi syndrome.
Feature- Lower limb deformity, stunted growth. Often with family history. Frequent dental abscess and early decay. Low serum phosphate and low TRP. Diagnosis – Familial hypophosphataemic rickets(FHR).
No clues so far, what else?
Features- Often presenting in early infancy. Hypocalcemic tetany. Improvement with vitamin D therapy and recurrence of symptoms on discontinuation. Diagnosis – vitamin D dependent rickets type1
Features-Alopecia with or without any response to any form of vitamin D High serum levels of 1,25 dihydroxy vitamin D. Diagnosis – vitamin D dependent rickets type2– 1,25(OH)2 vit D level is high in contrast to VDDR type 1 where it is low.
Further Investigations
• Gamma GT- 22
• iPTH- 8.9 (7.5- 53.5)
• 24 hr urinary Ca- 4.9 (1.25-6.25mmol/L)
• 24 hr urinary P-194.9 (Male: 360 – 1600 ,Female: 170 – 1200)
Endoscopy- no varices, Normal
Impression-
1. Hypophosphatemic Rickets- hereditary hypophosphatemic rickets with
hypercalciuria, Xlinked Hypophophatemic rickets
2. Phosphorus Deficiency- almost impossible to have a diet that is deficient in phosphorus, because phosphorus is present in most food.
3. Rickets 2ndary to Liver Disease
HHR with Hypercalciuria
( AR disorder- h/o consanguinity)
defect in gene for a sodium-phosphate cotransporter in the proximal tubule.
Clinical Manifestations – The dominant symptoms are rachitic leg abnormalities, muscle weakness, and bone pain. Patients can have short stature, with a disproportionate decrease in the length of the lower extremities. The severity of the disease varies, and some family members have no evidence of rickets but have kidney stones secondary to hypercalciuria
Laboratory Findings – hypophosphatemia, renal phosphate wasting, elevated serum alkaline phosphatase levels, and elevated 1,25-D levels. PTH levels are low.
Familial Hypophosphatemic Rickets – A Case Report and Review of Literature-MD. SHAHIDUL HAQUE1 Bangladesh JCH – XLH must be considered as a differential diagnosis with any form of rickets, who has positive family history, presence of bowing of legs, knock knee, coxa vara, genu varum (rather than Harrison’s sulcus, rachitic rosary or myopathy), hypophosphatemia with corresponding phosphaturia and normal serum PTH level.
• However, renal, hepatic or other related causes should also be excluded as differential diagnosis.
In our patient here, USG was suggestive of Cirrhosis
Evaluation – Cause of Cirrhosis? And we needed to confirm cirrhosis.
Etiology and Complications of Liver Cirrhosis in Children: Report of a Single Center from Southern Iran, Seyed Mohsen Dehghani1
A total of 106 cirrhotic children aged between 5 months to 18 years with a mean age of 8.24 ± 6.12 years that included 60 boys (56.6%) and 46 girls (43.4%) were enrolled in the study.
Causes found out were
The most common causes of liver cirrhosis were
1. Wilson disease (n=22; 20.7%), Mean age 6-18 yr
2. biliary atresia (n=19; 17.9%), and
3. crypto- genic cirrhosis (n=14; 13.2%).
4. autoimmune hepatitis (n=12;11.3%)
5. idiopathic neonatal hepatitis (n=10; 9.4%)
6. hepatorenal tyrosinemia (n=9; 8.5%),
7. glycogen storage disease (n=6; 5.7%), and
8. progressive familial intrahepatic cholestasis (n=4;
3.8%).
Back to Our Case
Further Evaluation
• Ophthalmology Consultation- BE myopic astigmatism, Kascher-feischer Ring
• HBsAg, HCV serology- NR
• Serum Ceruloplasmin- 16 ( 20-30)
• 24 hrs urinary copper- 304 microgram/L ( 20-50)
• Liver Biopsy was done
FINAL DIAGNOSIS
Liver Biopsy Confirmed Cirrhosis, tissue sent for PAS and Trichome stains
Dx- Wilson’s Disease with hepatic
Cirrhosis with refractory Rickets
TREATEMENT started-
Tab Penicillamine-d 500 mg PO BD Tab Zinc-DT 30mg PO TDS
Advised to avoid high copper containing diets
Family screening for Wilson advised. F/U.
Now,
Tying up – Can Wilson Disease explain all findings?
Can rickets be a presenting feature in Wilson’s disease?
– If yes, why??? Mechanisms….
• Can Cirrhosis be a result of Wilson’s disease
• Can Hypercalciuria and nephrolithiasis be a manifestation of Wilson disease
We searched for case reports-
Similar case Reports-
Case I Gastroenterology Research • 2011;4(1):34-35 Wilson’s Disease Presenting as Resistant Rickets
Case II Vitamin D – Resistant Rickets as Presenting Feature of Wilson’s Disease- JIACM 2004; 5(3): 277-80
Case III Nephron. 1993;65(3):460-2. Hypercalciuria and nephrocalcinosis, a feature of Wilson’s disease.,Hoppe B et al
Our Patient initially had h/o hematuria and was found to have hypercalciuria and hematuria before bony changes appeared before any Hepatic or Neuropsychiatric manifestations
Similarly few other case reports were found where Hypercalcemia and nephrocalcinosis were the early manifestations of later diagnosed Wilson Disease.
Progressive Cirrhosis – a frequent hepatic presentation of Wilson Disease
The most frequent mode of hepatic presentation of Wilson’s disease, however, is the development of progressive cirrhosis. The cirrhosis has no Wilson’s disease– specific features. Because of the varied modes of hepatic presentation that Wilson’s disease can assume, any individual younger age with unexplained liver disease should be screened for Wilson’s disease.
Brewer GJ. Wilson’s Disease: A Clinician’s Guide to Recognition, Diagnosis, and Management. Boston: Kluwer Academic Publishers; 2001
Hepatic Wilson Disease
• Forms of Wilsonian hepatic disease include
– asymptomatic hepatomegaly (with or without splenomegaly),
– subacute or chronic hepatitis, and
– acute hepatic failure (with or without hemolytic anemia).
• Cryptogenic cirrhosis, portal hypertension, ascites, edema, variceal bleeding, or other effects of hepatic dysfunction (delayed puberty, amenorrhea, coagulation defect) can be manifestations of Wilson disease. Disease presentations are variable, with a tendency to familial patterns.
• The younger the patient, the more likely hepatic involvement
will be the predominant manifestation.
Conclusion
Rickets presenting at late childhood, non-nutritional causes should be thought for.
Wilsons disease may have many forms of atypical presentations and manifestations can be variable.
It should always be a differential in any unexplained liver disease, cirrhosis in young patients, neurological manifestations , forms of refractory rickets and unexplainable renal manifestations.