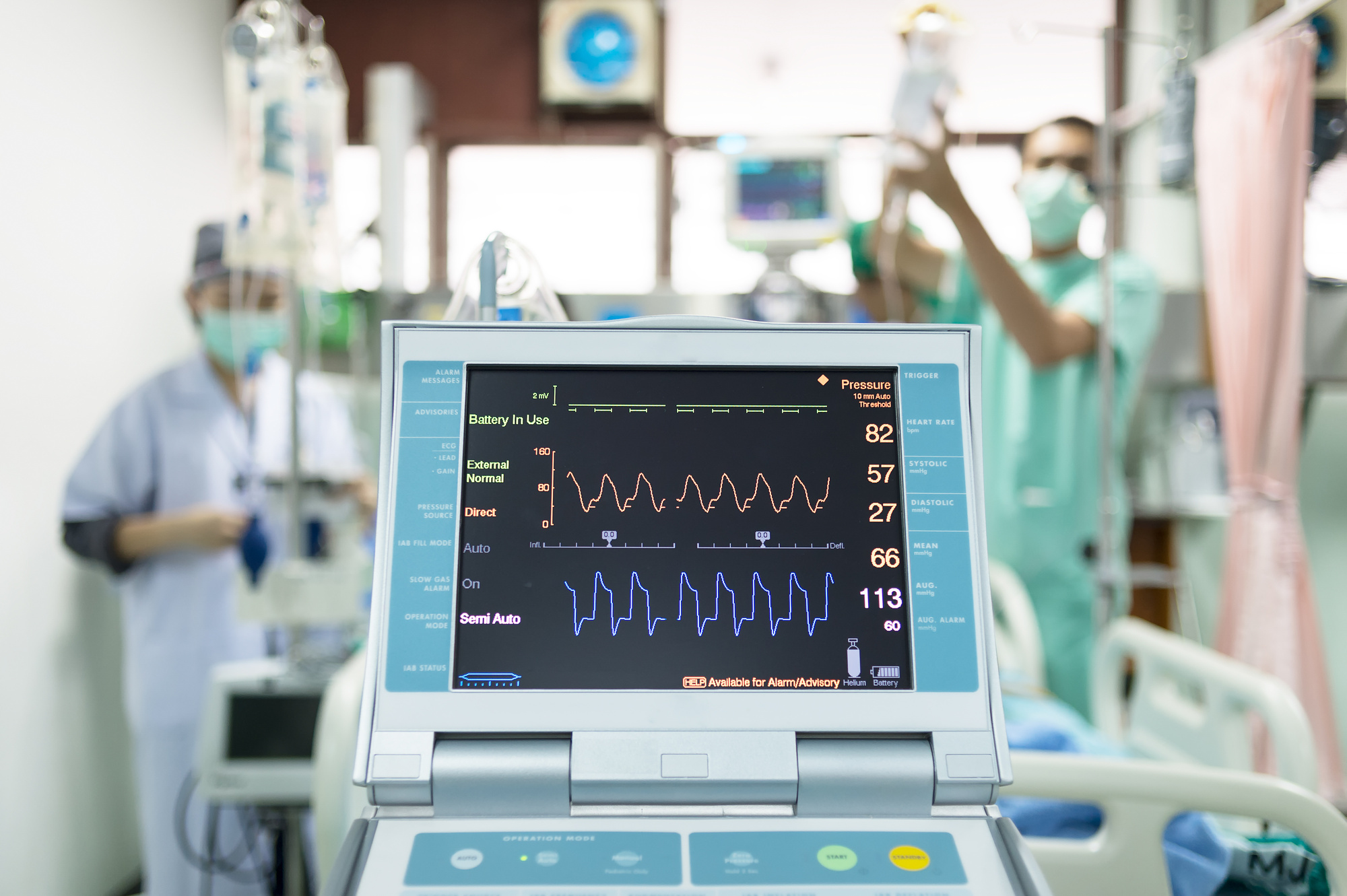
The Importance Of Value-Based Critical Care
In healthcare, critical care signifies an area of immense significance and sensitivity. With patients needing intensive monitoring and treatment, the approach adopted in critical care settings can profoundly impact patient outcomes.
Among the array of methodologies and principles that steer critical care, one concept that deserves special attention is value-based critical care.
This article aims to elucidate the importance of embracing value-based care in critical care settings and how it can optimize outcomes for patients and healthcare systems.
Redefining Care in the Intensive Care Unit
Patients in the intensive care unit (ICU) often battle life-threatening conditions requiring specialized care and attention. The traditional focus in the ICU has been on providing the highest level of medical interventions to sustain life.
However, the paradigm is shifting towards integrating value as a core care component. The value-based approach examines the balance between the quality of care and the costs involved, emphasizing patient-centered outcomes.
The Significance of Value-Based Critical Care
To understand the significance of value-based critical care, here are several key aspects that highlight its importance:
- Maximizing Patient Outcomes
Value-based critical care is pivotal in ensuring patient outcomes are at the forefront of care decisions. Concentrating on the patient’s needs and preferences, this approach aims for the most favorable results, considering physical health and psychological and emotional well-being.
It recognizes that every patient has unique values, goals, and expectations. By incorporating patient-centered care principles, value-based critical care promotes shared decision-making, where healthcare providers collaborate with patients to develop individualized care plans.
This personalized approach considers the patient’s cultural background, personal beliefs, and social support systems, ultimately improving patient outcomes and overall satisfaction.
Through close attention to patients’ holistic well-being, value-based critical care strives to treat diseases and injuries and enhance the overall quality of life for patients in the intensive care unit.
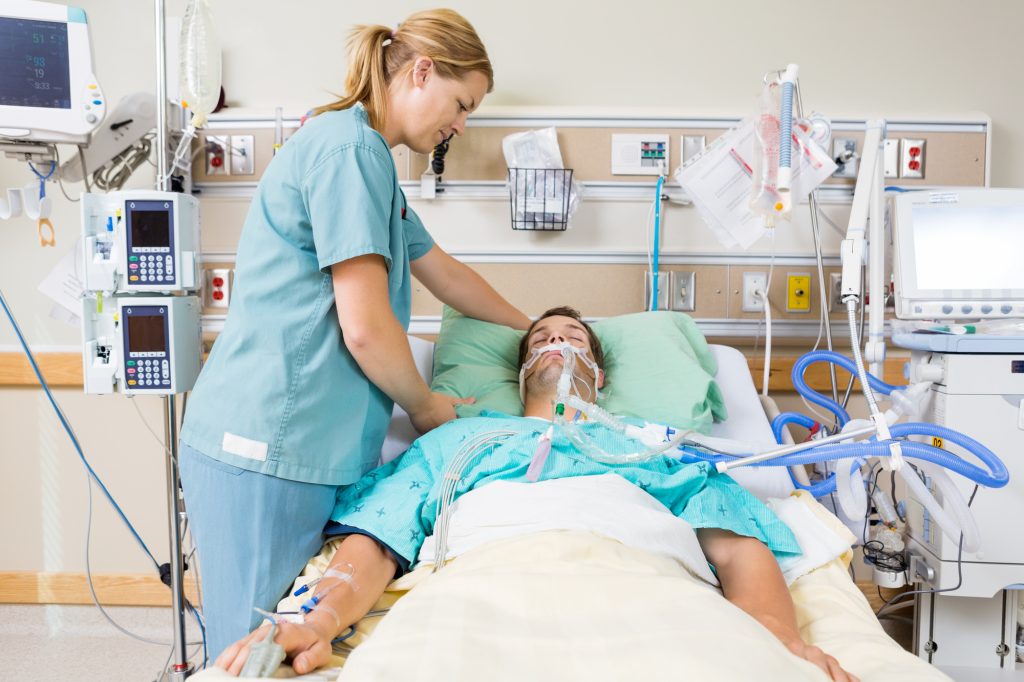
- Enhancing Patient Satisfaction
An intrinsic component of value-based critical care is the patient’s satisfaction. When the care provided aligns with patients’ values and preferences, it enhances their satisfaction. It, in turn, can positively influence their engagement and adherence to treatment plans.
This approach recognizes that patient satisfaction goes beyond clinical outcomes and encompasses communication, respect, and the ability to participate in their care actively.
When patients feel heard, respected, and empowered in their healthcare journey, they’re more likely to be satisfied and motivated to collaborate in their treatment. It can improve treatment adherence, reduce complications, and improve health outcomes.
- Optimizing Resource Allocation
In value-based critical care, another crucial aspect is the optimization of resource allocation. By prioritizing the efficient and effective use of resources, value-based care seeks to ensure that patients receive the necessary care without incurring excessive expenses while maintaining the highest quality of care.
This method is crucial in healthcare systems where resource constraints are common and the high demand for critical care services.
Here are some key points that highlight the importance of optimizing resource allocation in value-based critical care:
- Cost-Effective Interventions: Value-based critical care focuses on identifying and implementing interventions that provide the best outcomes for the cost incurred. It involves assessing the cost-effectiveness of various treatments and interventions and considering alternatives that offer comparable benefits at a lower cost.
- Avoidance of Unnecessary Tests and Procedures: Unwarranted tests and procedures contribute to healthcare costs and can increase the risk of complications for patients. Value-based critical care emphasizes the judicious use of tests and procedures, ensuring they’re necessary and aligned with the patient’s condition and care goals.
- Efficient Resource Utilization: Value-based critical care encourages healthcare providers to use resources efficiently within the ICU. It includes optimizing staffing levels, ensuring appropriate utilization of equipment and supplies, and minimizing waste. Streamlining processes and eliminating unnecessary steps or redundancies can direct resources where needed.
It’s important to note that optimizing resource allocation in value-based critical care doesn’t mean compromising the quality of care or denying necessary treatments.
Instead, it encourages healthcare providers to critically evaluate the utilization of resources and make evidence-based decisions that maximize patient outcomes while ensuring cost-effectiveness.
- Encouraging Preventive Care
Value-based critical care significantly emphasizes preventive measures to mitigate the need for intensive care. By focusing on early interventions and promoting overall health, value-based care aims to prevent escalating conditions that may require critical care interventions.
This approach involves proactive measures such as health screenings, patient education, lifestyle modifications, and immunizations. Value-based critical care aims to reduce the incidence and severity of illnesses, ultimately lowering the burden on intensive care units and improving population health.
- Improving Communication and Collaboration
Effective communication and collaboration are paramount in value-based critical care to ensure coordinated and patient-centered care. It involves open and clear lines of communication among healthcare professionals within the interdisciplinary team, enabling a seamless exchange of information and expertise.
Furthermore, value-based care emphasizes meaningful engagement with patients and their families, involving them in decision-making and considering their values, preferences, and care goals.
This collaborative approach fosters trust, enhances patient satisfaction, improves treatment adherence, and allows for shared decision-making that aligns with the patient’s needs and values.
- Ensuring Ethical Standards
Value-based critical care integrates ethical considerations into care decisions to ensure the provision of morally responsible healthcare. It involves upholding principles such as patient autonomy, which respects patients’ right to be actively involved in their care and make informed decisions.
Beneficence, the obligation to act in the patient’s best interest, guides value-based care to prioritize interventions that maximize patient outcomes. Justice plays a role in equitable resource allocation and ensuring fair access to critical care services.
By adhering to these ethical standards, value-based critical care ensures that it’s clinically appropriate, aligns with the patient’s values, and respects their autonomy.
- Utilizing Data-Driven Decision Making
Value-based critical care leverages data analytics to inform decision-making processes and continuously improve the quality of care. By analyzing patient records, clinical outcomes, and research findings, healthcare providers can provide valuable insights to guide their treatment strategies.
This data-driven approach identifies best practices, evaluates interventions, and monitors patient outcomes.
By employing evidence-based practices supported by robust data analysis, value-based critical care enhances the effectiveness and efficiency of care delivery, optimizing patient outcomes and resource utilization.
- Facilitating Continuous Improvement
Value-based critical care fosters a culture of continuous improvement by regularly assessing care processes, seeking feedback, and implementing evidence-based practices. Through ongoing evaluations of patient outcomes, protocols, and performance indicators, healthcare professionals and systems can identify areas for improvement and implement necessary changes.
This commitment to continuous improvement promotes learning, innovation, and the implementation of best practices, ensuring that care delivery is always evolving better to meet patients’ needs in the critical care setting.
By striving for constant enhancement, value-based critical care supports delivering high-quality, patient-centered care.
- Promoting Patient Safety
Ensuring patient safety is a fundamental aspect of value-based critical care. By prioritizing patient safety, this approach aims to prevent adverse events, medical errors, and complications that can arise during critical care interventions.
Here are key points that highlight the importance of promoting patient safety in value-based critical care:
- Adherence to Evidence-Based Guidelines: Value-based critical care promotes the consistent implementation of evidence-based guidelines and protocols designed to enhance patient safety and minimize the risk of harm. By following established best practices, healthcare providers can reduce variability in care delivery and ensure a standardized, safe approach.
- Robust Medication Management: Medication safety is critical to patient care in the intensive care unit. Value-based critical care emphasizes medication reconciliation, clear communication about medications, and adequate monitoring to prevent medication errors and adverse drug events.
- Infection Prevention and Control: The risk of healthcare-associated infections is high in the intensive care unit. Value-based critical care emphasizes infection prevention and control measures, including proper hand hygiene, aseptic techniques, appropriate use of personal protective equipment, and timely implementation of infection control protocols.
- Error Reporting and Learning Culture: Value-based critical care encourages the development of a culture of safety that fosters open communication, encourages error reporting, and promotes learning from adverse events or near misses.
- Patient Monitoring and Surveillance: Value-based critical care emphasizes using advanced monitoring technologies to detect changes in patient conditions promptly. Continuous monitoring of vital signs, electronic health record alerts, and real-time surveillance systems enable healthcare providers to identify potential risks or deteriorations early, allowing for timely interventions and preventing adverse outcomes.
By focusing on patient safety through adherence to evidence-based guidelines, robust medication management, infection prevention, and control, fostering a culture of reporting and learning from errors, and implementing comprehensive patient monitoring, value-based critical care ensures the highest level of safety for patients in critical care settings.
Conclusion
In conclusion, value-based critical care is a transformative approach that prioritizes patient outcomes, efficient resource utilization, and patient-centered, ethical care. By emphasizing effective communication, preventive measures, and continuous improvement, value-based critical care enhances the quality of care provided in critical settings.
Readers who engage with this article gain valuable insights into embracing value-based care in critical care settings and how it can optimize outcomes for patients and healthcare systems.
Implementing the principles discussed can improve patient satisfaction, resource allocation, and overall healthcare quality. Take the first step toward value-based critical care and start reaping the benefits today.
Allen John Smith
Allen John Smith is an experienced healthcare writer passionate about promoting value-based critical care. With a deep understanding of the field and a commitment to patient-centered approaches, Allen’s articles provide valuable insights and inspire positive change in the industry. When he’s not writing, Allen can often be found hiking scenic trails, exploring nature, or capturing breathtaking landscapes through his photography. His love for the outdoors fuels his creativity and inspires him to advocate for holistic well-being in healthcare.