Lumbar Stenosis: Symptoms, Diagnosis, Treatment, And Recovery
Back pain resulting from lumbar stenosis is a common problem among older adults—but it also afflicts younger people. Lumbar stenosis is when the spinal canal in the lower back becomes narrowed, putting pressure on the spinal cord and nerves. The pressure then causes a painful sensation that can be felt in the back and all the way to the buttocks and legs.
Lumbar stenosis can be caused by various factors, including degeneration of the spine due to aging or injury, persistent carrying of heavy load, obesity, abnormal growths, spinal deformity, genetic disease, and herniated discs.
The pain ranges from mild to excruciating and is aggravated by movement. It can persist and cause disability or poor performance at work.
Back Pain: A Common Ailment
Back pain is more common than you think, but not all back pain is due to lumbar stenosis. Many people complain of back pains, and some cases usually require a trip to the emergency room.
Nine out of ten people reported having back pain at least once, and 39% of adult Americans complained that they experienced back pain for the last three months.
Studies also find that back pain affects more women than men, especially among seniors. This could be due to the damage acquired during pregnancy, osteoporosis, or sudden weight gain during menopause. Even carrying babies or heavy loads strains the back.
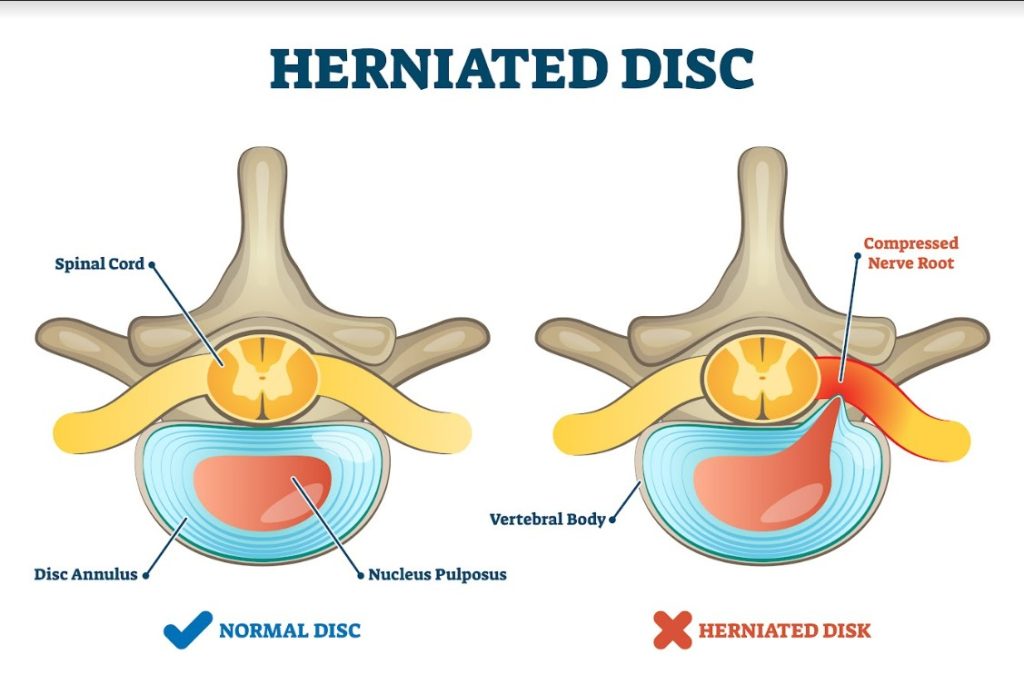
Symptoms of Lumbar Stenosis
Lumbar stenosis is a condition where the spinal canal in the lower back or lumbar region narrows. Because of the small space, the pressure on the spinal cord and nerves increases. Symptoms may gradually develop over time or come on suddenly and be severe. They may be present all the time or only when the person is standing or walking.
Symptoms of lumbar stenosis can vary depending on the condition’s severity and the nerves being compressed. This pressure can cause pain, numbness, tingling, and weakness in the legs, buttocks, and lower back. It can even cause paralysis.
The pain due to lumbar stenosis, often described as an aching or burning feeling, radiates to the buttocks and behind the legs. It also causes difficulty in walking—sometimes manifested by the heaviness of the legs or dragging. Occasionally, patients can experience a sudden onset of cramps while walking.
Low back pain can also be aggravated by prolonged standing or walking. It is relieved by sitting, bending forward, or flexing the foot. Incontinence or loss of bladder and bowel control is rare but usually occurs in severe cases. In Idaho, laminectomy or foraminotomy is the surgery typically done at dickinsonneurosurgery.com to provide relief, especially when oral medications and other non-surgical interventions offer no comfort.
It’s important to note that not everyone with lumbar stenosis will have symptoms, and these could vary if the patient has an underlying condition. In other cases, the initial complaints are difficulty walking or standing for long periods. If the symptoms are severe and progressive, it is essential to consult a doctor.
The symptoms can progress over time and may lead to difficulty performing daily activities. Depending on how much of the spine is affected, stenosis can cause neck stiffness, headaches, and lower limb problems. However, those with mild symptoms can be managed with conservative treatment.
When To See A Doctor?
Back pain is commonly experienced by adults, especially those who are frequently stressed from their job. Common back pain can be relieved with enough rest and other natural methods such as exercise and proper posture. However, if the pain gradually increases and becomes unbearable, it could be time for a medical checkup.
If your back pain is consistently progressing and it is coupled with the symptoms that are mentioned above, then it’s best to consult your doctor as soon as possible. Make sure your doctor checks for lumbar stenosis so you can start a treatment plan immediately.
Diagnosis
Diagnosing lumbar stenosis typically begins with a detailed medical history and physical examination. The doctor may ask about the patient’s symptoms, including when they started, how often they occur, how severe they are, and what aggravates the condition.
The doctor may also perform a neurological examination to check for any nerve damage or compression signs. During the physical examination, the healthcare provider will check for signs of muscle weakness, loss of reflexes, and sensory changes. Sensory changes mean fine touch perception, pressure, and temperature loss.
They will also look for any structural spine changes that could contribute to the stenosis, such as a herniated disc or a bony spur. Imaging tests are often used to confirm the diagnosis and determine the extent of the stenosis. Tests like x-rays, CT scans, or MRI scans can show the spine’s structure, including any degenerative changes or abnormal growths (e.g., cancer) that may be causing the stenosis.
Sometimes, your doctor may perform additional tests, such as a myelogram, a particular type of x-ray that uses a dye. These tests can provide detailed images of the spine and show any narrowing of the spinal canal or compression of the nerves.
An electromyography (EMG) test is ordered if nerve compression is entertained. These tests measure the electrical activity in the muscles and nerves and can help to determine if a nerve is being compressed. In some cases, doctors may order a lumbar puncture for further evaluation.
Your doctor may recommend a treatment plan such as physical therapy, medications, or surgery based on the diagnosis. Not all lumbar stenosis requires surgery, and a multidisciplinary approach is often the best way to manage the condition.
Treatment
The treatment of lumbar stenosis typically depends on the severity of the condition and the specific symptoms the patient is experiencing. Pain relief and improvement in the patient’s ability to function are the goals of treatment.
Treatment for lumbar stenosis typically starts conservatively with non-surgical solutions and may include the following:
- Physical therapy, which includes exercises that help strengthen the muscles in the back and legs and to improve flexibility and balance
- Medications that could include non-steroidal anti-inflammatory drugs (NSAIDs) or pain relief medications and muscle relaxants to help manage pain and inflammation.
- Epidural steroid injections to reduce inflammation and pain
- Lumbar bracing, which reduces pressure on the nerves and provides support and stability to the lower back.
Ultimately, when the pain is progressive or intractable, surgery is performed. Though patients are wary because of the thought that their condition will worsen, surgery is often a definitive solution. Laminectomy relieves the spinal cord of pressure when the lamina or back part of the spinal cord is removed. Foraminotomy or spinal decompression removes bone or soft tissue.
It’s important to follow your doctor’s advice and regularly go to doctor’s appointments to monitor the progression of the disease and adjust the treatment as needed.
Recovery
The recovery process from lumbar stenosis can vary depending on the treatment received. The age and pre-existing condition of the patient can also affect the prognosis.
Recovery may take several weeks to months for patients who have undergone non-surgical treatments such as physical therapy, medications, or epidural steroid injections. Physical therapy and exercises can help the patient regain strength and mobility. During this time, it is crucial to follow the physical therapy plan as directed by the healthcare provider and to continue with any medications or other treatments as prescribed.
For patients who have undergone surgery, recovery can be longer. After surgery, patients may need to rest for several weeks to allow the surgical wounds to heal. They will then begin physical therapy and rehabilitation exercises to help regain strength, flexibility, and mobility. Full recovery can take several months and sometimes up to a year.
For those who have undergone non-surgical treatment such as physical therapy, recovery may take several weeks to several months. For those who have undergone surgery, healing can take longer, usually several months. It is essential to follow the postoperative instructions given by the surgeon, including any physical therapy or rehabilitation programs.
It’s important to note that recovery from lumbar stenosis may be gradual, and the patient should only do so slowly. Losing weight and maintaining good posture—even without medication or surgery—can significantly reduce pain.
Conclusion
Back pain can be scary and debilitating. While it may be caused by stress and lack of rest, serious conditions can also be behind it. Lumbar stenosis is one of the causes of back pain. While the elderly are more prone to this condition, younger adults can also be afflicted. The pain can be felt all throughout the buttocks, and in severe cases, the patient may have difficulty walking or standing.
The most common causes of lumbar stenosis are trauma, growth, scoliosis, herniated disk, and chronic weight bearing on the spine. Treatment can be non-surgical or surgical. However, a multidisciplinary approach works best. This means that surgery must be coupled with therapy and other relief medications to ensure proper treatment.
Recovery is possible, but patients should realize that progress may be slow. Age and pre-existing medical conditions are huge factors that can affect the recovery of the patient. Since most people who are diagnosed with lumbar stenosis are senior adults, recovery can typically take months or a year.