Hepatitis C Genotyping: Therapeutic Implications
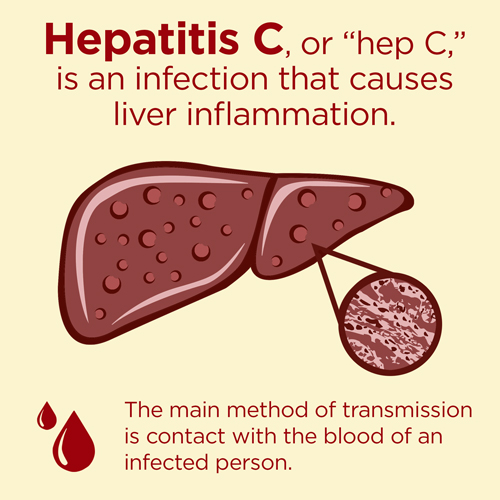
The hepatitis C virus (HCV) is a RNA virus belonging to the Flaviviridae family which causes viral hepatitis, a systemic infection affecting predominantly the liver and causing its inflammation and resulting in impaired liver function. The hepatitis C virus is a bloodborne virus and the most common modes of infection are through unsafe injection practices, inadequate sterilization of medical equipment, and the transfusion of unscreened blood and blood products.
Infection with HCV may present as acute hepatitis, but may progress to cause persistent chronic infection in a subset of those infected, with symptoms ranging in severity from a mild illness lasting a few weeks to a serious, lifelong illness. About 15–45% of infected persons spontaneously clear the virus within 6 months of infection without any treatment. The remaining 55–85% of persons will develop chronic HCV infection. Of those with chronic HCV infection, the risk of cirrhosis of the liver is between 15–30% within 20 years. In the absence of cofactors like heavy alcohol consumption or other liver diseases, chronic hepatitis C disease is characterized by slow progression leading to liver cirrhosis and its sequelae typically after 20–30 years after infection.
Worldwide, an estimated 130-150 million persons have chronic HCV infection. Approximately 700,000 persons die each year from HCV related complications, which include cirrhosis, hepatocellular carcinoma (HCC) and liver failure. HCV infection can be cured by antiviral treatment; however, due to the asymptomatic nature of the disease, many infected persons are unaware of their infection and, for those who are diagnosed, access to treatment remains poor in many settings. As the majority of infections took place before the discovery of the virus, it is now seen in many countries increasing numbers of patients who present with late stages of the disease. Thus, highly effective antiviral therapy is urgently required for many patients.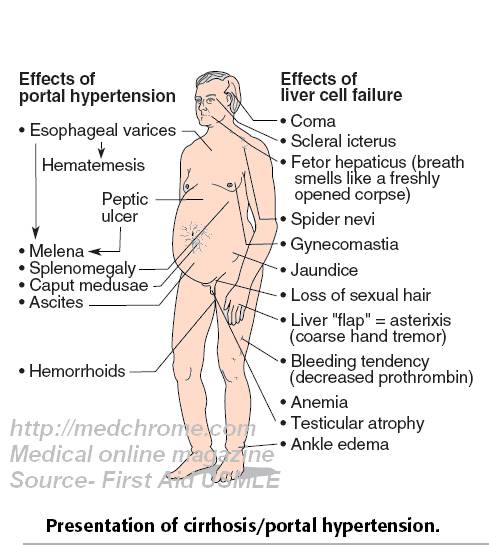
Screening and diagnosis
Due to the fact that acute HCV infection is usually asymptomatic, few people are diagnosed during the acute phase. In those people who go on to develop chronic HCV infection, the infection is also often undiagnosed because the infection remains asymptomatic until decades after infection when symptoms develop secondary to serious liver damage.
HCV infection is diagnosed in 2 steps:
- Screening for anti-HCV antibodies with a serological test identifies people who have been infected with the virus.
- If the test is positive for anti-HCV antibodies, a nucleic acid test for HCV ribonucleic acid (RNA) is needed to confirm chronic infection because about 15–45% of people infected with HCV spontaneously clear the infection by a strong immune response without the need for treatment. Although no longer infected, they will still test positive for anti-HCV antibodies
After a person has been diagnosed with chronic hepatitis C infection, an assessment of the degree of liver damage (fibrosis and cirrhosis) by liver biopsy or through a variety of non-invasive tests is done.In addition, these people should have a laboratory test to identify the genotype of the hepatitis C strain. The degree of liver damage and virus genotype are used to guide treatment decisions and management of the disease.
Impact of genotype on response to treatment:
HCV has a highly variable genome, which has been classified into six distinct genotypic groups based on genomic sequence variation and further divided into several subtypes. These genotypes respond differently to treatment, making it imperative to test for the genotype before treatment initiation. PCR sequencing methodology remains the gold standard for determining the HCV genotype.The distribution of HCV genotypes and subgenotypes varies substantially in different parts of the world; genotype 1 is the most common, accounting for 46.2% of all HCV infections, followed by genotype 3 (30.1%). The diversity of genotypes also varies; with the highest diversity observed in China and South-East Asia.HCV genotype 4 was found in the Middle East and North Africa, and genotypes 5 and 6 in South Africa and Asia, respectively.
Genotype identification is clinically important for prediction of responses to, and in determining the duration of, antiviral therapy. This is illustrated by the fact that genotypes 1 and 4 were more resistant to treatment with pegylated interferon-α and ribavirin than genotypes 2, 3 and 6. Patients with chronic HCV genotype 1b infection showed more severe liver disease than patients infected with other genotypes.
A study done from India (SRL Ranbaxy, 2002) showed a high prevalence of genotype 3 (> 76%), with genotype 3a to be the highest (50%) followed by 3b (25%). Genotype !b was found to be approximately 14% followed by 1a( 10%).A minimal number (approximately 4%) of genotype 4 was found only in Southern and Western India.
Therapy:
The goal of therapy is to cure HCV infection to prevent hepatic cirrhosis, decompensation of cirrhosis, HCC, severe extra-hepatic manifestations and death.The endpoint of therapy is undetectable HCV RNA (sustained virological response,SVR) in a sensitive assay (≤15 IU/ml) 12 weeks and 24 weeks after the end of treatment.
The standard treatment was the combination of pegylated interferon (PegIFN)-alpha and ribavirin for 24 or 48 weeks was the approved treatment for HCV infections.This regimen proved to be relatively ineffective with a viral eradication rate of approximately only 50%. Furthermore, interferon alfa-based antiviral therapy is associated with a number of severe adverse events, which excluded up to 50% of patients upfront from antiviral therapy.
A dramatic improvement in HCV therapy followed the introduction of oral medicines that directly inhibited the replication cycle of HCV. These medicines, called direct-acting antivirals (DAAs), target three important regions within the HCV genome: NS3/4A protease, NS5A and NS5B RNA-dependent polymerase. These medicines have led to higher sustained virological responses (SVRs) than interferon-based regimens,are shorter in treatment duration, are orally administered and have fewer side-effects.Currently, five NS3 protease inhibitors (boceprevir, telaprevir,simeprevir, asunaprevir, paritaprevir), three NS5A inhibitors(daclatasvir, ledipasvir, ombitasvir), one non-nucleoside (dasabuvir)and one nucleotide NS5B inhibitor (sofosbuvir) are approved globally for treatment of chronic hepatitis C. Additional NS3 protease- (vaniprevir, grazoprevir, sovaprevir, ABT-493), NS5A- (elbasvir, velpatasvir/GS-5816, odalasvir/ACH-3102, ABT-530; MK-8408), non-nucleoside (beclabuvir, GS-9669) and nucleos(t)ide NS5B inhibitors (IDX-21437, ACH-3422) are in phase II–III clinical development.
Existing DAA treatments are significantly more effective on certain genotypes than others; thus, it is important to know a patient’s genotype prior to initiating treatment. New WHO guidelines in 2016 and European Association for the Study of the Liver (EASL) guidelines in 2015 reiterate the importance of determining the HCV genotype for optimising therapy. The HCV genotype and genotype 1 subtype (1a/1b) must be assessed prior to treatment initiation and will determine the choice of therapy as per the EASL guidelines in 2015. The choice and duration of therapy vary as per the genotype as detailed in the table below:
Source: WHO Guidelines for chronic hepatitis C, 2016
The first-generation DAAs that were marketed were the protease inhibitors boceprevir and telaprevir, which were co-administered with interferon and ribavirin. However, they were only effective in treating patients with genotype 1 infection; moreover, they caused frequent and sometime severe side-effects, particularly among persons with more advanced disease. The use of boceprevir- or telaprevir-containing regimens is no longer recommended for the treatment of HCV by the latest guidelines by EASL and WHO.
Second-generation DAAs have higher rates of SVR, are safer and can be used in combinations that obviate the need for interferon and ribavirin. Thus, these are referred to as “interferon-free” treatment regimens. The combination of two or three subclasses of these DAAs have demonstrated excellent efficacy in general, although cure rates among certain patient subgroups are lower.
To conclude,the field of HCV theraupetics continues to evolve rapidly, with several new medicines being approved in recent years. DAAs are transforming the treatment of HCV, enabling regimens that can be administered orally, are of shorter duration (as short as eight weeks), result in cure rates higher than 90%, and are associated with fewer serious adverse events than the previous interferon containing regimens. Determining the HCV genotype plays a crucial role in initiating appropriate therapy.
References:
- WHO | Hepatitis C http://www.who.int/mediacentre/factsheets/fs164/en/# 3/7 (accessed on 20.7.16)
- Nakamoto, Shingo, et al. “Antiviral therapies for chronic hepatitis C virus infection with cirrhosis.” World J Hepatol 7.8 (2015): 1133-1141.
- Cai, Qingxian, et al. “Comparison of three different HCV genotyping methods: core, NS5B sequence analysis and line probe assay.” International journal of molecular medicine 31.2 (2013): 347-352.
- Sarrazin, Christoph. “The importance of resistance to direct antiviral drugs in HCV infection in clinical practice.” Journal of hepatology 64.2 (2016): 486-504.
- European Association for the Study of the Liver. EASL recomendations on treatment of hepatitis C. J Hepatol. 2015;63(1):199–236.
- Guidelines for the screening, care and treatment of persons with chronic hepatitis C infection. Geneva: World Health Organization; 2016 (http://apps.who.int/iris/bitstream/10665/205035/1/9789241549615_eng.pdf, accessed 22 July 2015).
- Das, B. R. et al. “Geographical distribution of hepatitis C virus genotypes in India.” Indian Journal of Pathology & Microbiology 45.3 (2002): 323-328.
Author Profile

Research Scientist, SRL, R&D
SRL Ltd, Mumbai Reference Lab

President-Research & Innovation,
Mentor-Molecular Pathology and
Clinical Research Services
SRL R&D, Mumbai