Rules Mnemonics in Anatomy
All are about 45 cms or 18 inches:
- Length of Vas deferens or ductus deferens
- Length of thoracic duct
- Length of Spinal cord
- Femur (for 6 feet person)
- Length of transverse colon
- Distance from the incisor teeth to the cardiac end of the stomach
- Umbilical cord at birth
- Length of sartorius muscle
All are about 25 cms or 10 inches:
- Length of Esophagus
- Length of Ureter
- Length of Duodenum
- Length of Descending colon
All are about 10 cms or 4 inches:
- Length of Trachea
- Length of Fallopian or Uterine tube
- Length of Common bile duct
- Length of 3rd part of Duodenum (Transverse Duodenum)
- Length of Posterior wall of Vagina
- Anteroposterior measurement of Inlet of Pelvis
- Transverse measurement of Outlet of Pelvis
All are about 4 cms or 1.5 inches:
- Length of Auditory tube
- Length of Anal canal
- Length of Female urethra
- Length of Cystic duct
- Length of Common hepatic duct
- Length of External acoustic/auditory meatus when measured from tragus
- Length of Optic nerve
- Length of Ovary
- Length of Inguinal canal
- Length of Femoral sheath
- Thickness of Kidney
- Width of Pons
All are about 1 inch or 2.5 cm
- Length of Medulla
- Length of Midbrain
- Length of Pons
- Length of 4th part of Duodenum (Ascending Duodenum)
- Length of Ducts of Bartholin’s gland (Greater vestibular glands)
- Diameter of Trachea
- Diameter of Right main bronchus
- Distance between Ureteric orifice in Empty bladder
Structures whose width is greater than length:
- Pons varioli
- Cecum
- Prostate
Descent of Testis:
- 3rd month: Reaches Iliac fossa
- 6th month: Rests at Deep Inguinal ring
- 7th month: Traverses Inguinal canal
- 8th month: Reaches Superficial Inguinal ring
- 9th month: Descneds into Scrotum
Rule of 2s for Meckel’s Diverticulum:
Meckel’s Diverticulum is a congenital outpouching of the ileum that is a normal variant and is the remnant of omphalomesenteric (vitellointestinal) duct. It is a true diverticulum, that consists of all the layers of the intestinal wall (mucosa, submucosa and muscularis).
- Occurs in 2% population
- 2 times more common in male
- 2 feet proximal to ileocecal valve
- 2 inches in length
- 2 years of age is typical for onset of symptoms
- 2 % are symptomatic
- 2 types of mucosa possible (Small intestine and Gastric)
Rule of 2s: 2nd week of Development (Embryology)
- Trophoblast differentiates into 2 layers: Cytotrophoblast and Sycytiotrophoblast
- Embryoblast forms 2 layers: Epiblast and Hypoblast
- Extraembryonic mesoderm splits in 2 layers: Somatopleure and Splanchnopleure
- 2 cavities are formed: Amniotic cavity and Yolk sac cavity
Rule of 3s: Thoracic spine levelling
- T1-3 (and T12) transverse processes are at the level of the corresponding thoracic spine.
- T4-6 (and T11) transverse processes lie superiorly between its level’s spine and the spine of the thoracic segment above it.
- T7-9 (and T10) transverse processes lie superiorly at the level of the superior segment’s spine.
Rule of 3s: 3rd week of Development
- Bilaminar germ disc changes into trilaminar germ disc with 3 layers ectoderm, mesoderm and endoderm
- Formation of 3 important structures: Notochord, Neural plate and Primitive streak
- 3 layered chorionic villi
- 3 carnegie stages
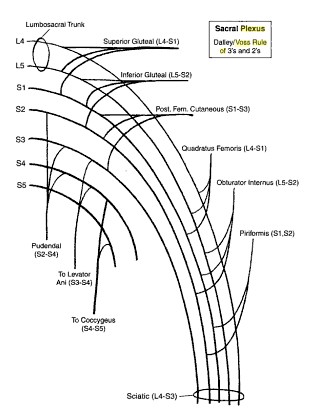
Dalley/Voss Rule of 3s of 2s: Sacral Plexus
- 1st set of 3 nerves will all have 3 spinal contributions (3,3,3)
- 2nd set of will have 2 nerves with 3 spinal contributions and 1 nerve with 2 spinal contributions (3,3,2)
- 3rd set will have 1 nerve with 3 spinal contributions and 2 nerves with 1 spinal contribution (3,2,2)
1st set of nerves (3,3,3):
- Superior gluteal nerve: 3 spinal contributions beginning from L4 (L4,L5,S1)
- Inferior gluteal nerve: 3 spinal contributions beginning from L5 (L5,S1,S2)
- Posterior femoral cutaneous nerve: 3 spinal contributions beginning from S1 (S1,S2,S3)
2nd set of nerves (3,3,2):
- Nerve to Quadratus femoris: 3 spinal contributions beginning from L4 (L4,L5,S1)
- Nerve to Obturator internus: 3 spinal contributions beginning from L5 (L5,S1,S2)
- Nerve to Piriformis: 2 spinal contributions beginning from S1 (S1,S2)
3rd set of nerves (3,2,2):
- Pudendal nerve: 3 spinal contributions beginning from S2 i.e. where you left off with pyriformis (S2,S3,S4)
- Nerve to levator ani: 2 spinal contributions beginning from S3 (S3,S4)
- Nerve to coccygeus:2 spinal contributions beginning from S4 (S4,S5)
Gate’s Rule of 4s: For Detecting Brainstem Lesion
There are 4 rules in Rules of 4s:
- 4 structures in the “M“idline begins with “M“: Motor pathway (Corticospinal Tract), Medial Lemniscus, Medial longitudinal fasciculus, Motor nucleus and nerves (CN 3,4,6,12)
- 4 structures to the “S“ide begins with “S“: Spinothalamic, Spinocerebellar tract, Sensory nucleus of CN V, Sympathetic pathway
- 4 Cranial nerves in Each of:
- Medulla: 9,10,11,12
- Pons: 5,6,7,8
- Above Pons: 1,2,3,4
- The 4 midline motor nuclei can exactly divide 12 (excluding 1 and 2 which are purely sensory) – 3, 4, 6 and12 (Remaining 4 motor nuclei are on sides/laterally i.e 5, 7, 9 and 11).
Associated deficits of 4 Midline “M” structures:
- Motor pathway (or corticospinal tract): contralateral weakness of the arm and leg.
- Medial Lemniscus: contralateral loss of vibration and proprioception in the arm and leg.
- Medial longitudinal fasciculus: ipsilateral internuclear ophthalmoplegia (failure of adduction of the ipsilateral eye towards the nose and nystagmus in the opposite eye as it looks laterally).
- Motor nucleus and nerve: Ipsilateral loss of affected cranial nerve function (3, 4, 6 or 12).
Associated deficits of 4 Side “S” structures:
- Spinocerebellar pathways: ipsilateral ataxia of the arm and leg.
- Spinothalamic pathway: contralateral alteration of pain and temperature affecting the arm, leg and rarely the trunk.
- Sensory nucleus of 5th Cranial nerve: ipsilateral alteration of pain and temperature on the face in the distribution of the 5th cranial nerve (this nucleus is a long vertical structure that extends in the lateral aspect of the pons down into the medulla).
- Sympathetic pathway: Ipsilateral Horner’s syndrome i.e ptosis, miosis, anhydrosis.
Associated deficits of 4 Cranial nerves in Medulla:
- 9th or Glossopharyngeal: ipsilateral loss of pharyngeal sensation
- 10th or Vagus: ipsilateral palatal weakness
- 11th or Spinal accessory: ipsilateral weakness of the trapezius and sternocleidomastoid muscles
- 12th or Hypoglossal: ipsilateral weakness of the tongue
Associated deficits of 4 cranial nerves in Pons:
- 5th or Trigeminal: ipsilateral alteration of pain, temperature and light touch on the face back as far as the anterior two-thirds of the scalp and sparing the angle of the jaw
- 6th or Abducens: ipsilateral eye abduction weakness
- 7th or Facial: ipsilateral facial weakness
- 8th or Auditory: ipsilateral deafness
Associated deficits of 4 cranial nerves above Pons:
- 1st or Olfactory: not in midbrain.
- 2nd or Optic: not in midbrain.
- 3rd or Occulomotor: impaired adduction, supraduction and infraduction of the ipsilateral eye (eye is turned out and slightly down)
- 4th or Trochlear: eye unable to look down when the eye is looking in towards the nose
Applying the knowledge:
Pathways and tracts pass through the entire length of brainstem and can be likened to “meridians of longitude” whereas the cranial nerves can be likened to “parallels of latitude”. To establish the site of brainstem lesion, you need to detect the point of intersection of the meridians of longitude and parallels of latitude. Thus a medial brainstem syndrome will consist of the deficits of 4 “M”s and the relevant motor cranial nerve, and a lateral brainstem syndrome will consist of the deficits of 4 “S”s and either the 9–11th cranial nerve if in the medulla, or the 5th, 7th and 8th cranial nerve if in the pons.
Example:
58 years old lady with left hemiparesis, Left side loss of proprioception and right sided tongue deviation.
- Left hemiparesis is associated with deficit of Motor or corticospinal pathway of Right side which lies medially
- Left sided loss of proprioception is associated with deficit of medial lemniscus of Right side which lies medially
- Right sided tongue deviation is associated with deficit of Cranial nerve 12 on Right side which lies medially in medulla
Diagnosis: Medial medullary syndrome due to lesion in right vertebral artery
Rule of 7s: For Orbit
There are 7 bones, 7 intraorbital muscles and 7 nerves in orbit
- 7 Bones: Frontal, Ethmoid, Lacrimal, Sphenoid, Zygomatic, Palatine, Maxilla
- 7 intraorbital muscles: Levator palpebrae, 4 recti (Superior, Inferior, Medial and Lateral), 2 oblique (Superior and Inferior)
- 7 orbital nerves: Optic (CN II), Occulomotor (CN III), 3 branches of Opthalmic nerve (CN V1) – Frontal, Nasociliary, Lacrimal, Abducens nerve (CN VI)
- 9 % in head and neck
- 9% in each upper limb
- 18% in front of the trunk
- 18% in back of the trunk (including buttocks)
- 18% in each lower limb
- 1% in perineum
- 18% in head and neck
- 9 % in each limb
- 18% in front of the trunl
- 18% in back of the trunk
- 13.5% in each lower limb
- 1% in perineum

Trachea Length= 10 cm
Left bronchus= 5 cm
Right bronchus= 2.5 cm
Trachea width= 2.5 cm
Other structures whose width is greater than their length :
Coeliac trunk
Pituitary gland
Isthmus of thyroid
Very useful …
thank you so much !
Very useful and accurate. Good work!
wahhhh excellent