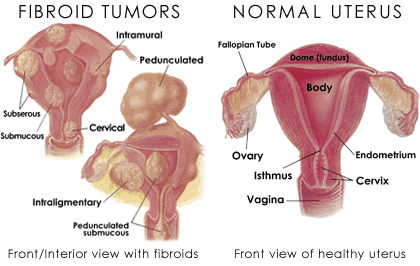
Uterine leiomyoma or Fibroid
Definition: Most common benign neoplasm of female genital tract composed of smooth muscle and connective tissue that is hormonally responsive (Growth ↑ in pregnancy and ↓ after menopause).
Gross pathology:
- Discrete, round, firm, irregularly lobulated and often multiple.
- Enlarged uterus
- Smooth and white cut surface with whorled appearance
- False capsule: pinkish color
- Center of tumor is least vascular and likely to degenerate
Risk factors:
- Nulliparity
- Obesity
- Hyperestrogenic state
- Black race
Types:
| Types | Features |
| Intramural | Within uterine wall |
| Subserosal | Projects into the pelvis à irregular uterine contour; may be pedunculatedWandering/Parasitic fibroid: Nourishment from omental/mesenteric adhesion |
| Submucosal | Projects into uterine cavity; irregular uterus; may be pedunculated |
| Cervical and Broad ligament | RarePseudocervical fibroid: Arising from uterine body & occupying cervical canal |
Secondary changes in fibroid:
- Degeneration: Hyaline (commonest), Cystic, Fatty (Myxomatous), Calcific (Womb stone), Atrophic
- Septic degeneration: Necrosis followed by infection
- Red degeneration (Carneous degeneration)
- During 2nd and 3rd trimesters of pregnancy, myomas may rapidly increase in size and undergo vascular deprivation and subsequent degenerative changes (aseptic degeneration and infarction)
- C/F: Pain and localized tenderness
- Complications: Preterm labor, DIC
- Venous thrombosis and congestion with interstitial hemorrhage is responsible for color
- Sarcomatous changes: Rare
History:
- Age: peak in 35-45 years
- Often asymptomatic (75%)
- Abnormal Uterine Bleeding:
- Cause: Increased vascularity and venous congestion, Increased surface area of uterine cavity
- Menorrhagia (Prolonged, heavy bleeding), Metrorrhagia (Intermenstrual bleeding), Premenstrual spotting and Anemia symptoms
- Pressure:
- Constipation (Intestinal obstruction), Urinary symptoms of hydroureter, Lower extremity edema (Pelvic venous congestion)
- Pain:
- Cause: Torsion, Degeneration, Protrusion (Myometrial contraction to expel submucosal myoma from uterine cavity)
- Secondary dysmenorrhea, Dyspareunia
- Sensation of heaviness or fullness in pelvic area with large tumor
- Infertility:
- Cause: Mechanical obstruction or distortion of uterine cavity interfere with implantation and sperm transport
Examination:
- Pallor (AUB)
- Abdominal examination:
- Palpation: If >14 wks size, firm/non-tender/irregular/mobile side-to-side only
- Percussion: Dull
- Peritoneal signs: Infarcted myoma
- Bimanual pelvic examination:
- No groove or separation of mass from uterus
- Cervix moves with movement of tumor felt per abdomen
- Exception: Subserous pedunculated fibroid often confused with ovarian mass
Uterine retroversion and retroflexion may obscure the physical examination diagnosis of even moderately large leiomyoma
Differential Diagnosis:
- Fetus (Pregnancy)
- Full bladder
- Adenomyosis
- Myohyperplasia
- Tubo-ovarian mass
- Ovarian tumor
Investigations:
- Lab: Anemia (Bleeding), Polycythemia (Erythropoietin induced by ureteral back pressure), Degeneration or Infection (Leukocytosis, Fever, Elevated ESR), Pregnancy test, CA-125 (Differentiating from other gynecologic adenocarcinomas)
- Imaging:
- Pelvic USG: To confirm diagnosis
- MRI: Can delineate intramural and submucous myomas (location); evaluate urinary tract
- Hysterosalpingography or Hysteroscopy: In infertile patient
- Laparoscopy: Helpful if uterine size < 12 wks
- AXR: Calcification, Preoperative assessment
- IVU: Anatomic changes in ureter
- D & C: Detect co-existing pathology in presence of uterine bleeding
Management:
1) Asymptomatic fibroid:
- Regular supervision @ 6 months interval
- Surgery: If size > 12 wks, Diagnosis uncertain, Unexplained infertility or abortion, Pedunculated fibroid, Size increase or symptoms appear
2) Symptomatic fibroid:
- Medications:
- Goal: To slow or stop bleeding, To decrease size of myoma, suppress further growth and reduce vascularity (as neoadjuvant therapy)
- GnRH agonists: Hypoestrogenic state
- Leuprolide (im), Nafarelin (intranasally), Goserelin (sc implant)
- GnRH antagonists: Cetrorelix, Ganireflix
- Progestogens: Medroxyprogesterone acetate 200mg im monthly; Norethindrone
- Antiprogesterones: Mifepristone 25-30 mg daily X 3 months
- Danazol 200-400 mg daily X 3 months
- Surgery:
- Indications:
- Medical therapy: Contraindication, Intolerance, Failure
- Concern for malignancy
- Mass effect: pain, pressure, urinary or GI symptoms
- Infertility, Repeated abortions
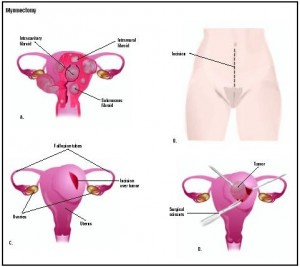 Modalities:
Modalities:
- Hysterectomy
- Definitive treatment with no chance of recurrence
- Indications: Extensive disease, suspected malignancy, Myomas is association with other pelvic abnormalities, Future pregnancy not desired
- Total or Subtotal hysterectomy (Ovaries can be removed in postmenopausal)
- Vaginal hysterectomy: can be done if size 10-12 wks associated with uterine prolapse
- Myomectomy: Preferred if future pregnancy desired
- Laparotomy: Multiple myomas or Uterus > 16 wks size
- Laparoscopy: 1-2 easily accessible myoma <8cm diameter and uterine size <16 wks
- Hysteroscopy +/- Endometrial ablation: Submucosal myomas 3-4 cm diameter
- Myolysis:
- Laparoscopy: Coagulation/Freezing of myoma
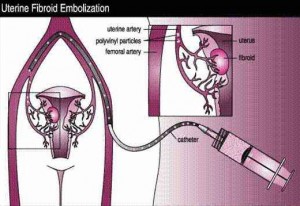
- Uterine artery embolization:
- Fluoroscopic guidance: Gels, beads, or coils through a catheter in common femoral artery
- Disrupts blood supply, causing degeneration
- Hysterectomy
- Indications:
-
-
- High-intensity focused ultrasound: Heat generation; Developmental stage
-
Causes of symmetrical enlargement of uterus:
- Pregnancy
- Submucosal or intramural fibroid for which you should visit Access Vascular
- Adenomyosis
- Myohyperplasia
- Metras: Pyo/Hemao/Lochio-metra
- Malignancy: Carcinoma body, Choriocarcinoma, Sarcoma